Category: Medicine and Pharmaceuticals
Malaria will soon be a notifiable disease across India
25, Apr 2023

Why in News?
- Malaria is all set to become a notifiable disease across India, with Bihar, Andaman and Nicobar Islands and Meghalaya too in the process of putting this vector-borne disease in the category.
About the News:
- This will then require by law that cases be reported to government authorities.
- Currently malaria is a notifiable disease in 33 States and Union Territories in India.
- Confirming the development, a senior Health Ministry official said this is part of India’s vision to be malaria-free by 2027 and to eliminate the disease by 2030.
- The Health Ministry has also initiated a joint action plan with the Ministry of Tribal Affairs for malaria elimination in tribal areas.
What happens when a disease is put under “Notified” Category?
- The doctors have to report about the occurrence of disease in their patients to the Chief Medical Officer of the district.
- It will help authorities to collect information of the spread of the disease, monitor the disease and set off early warnings.
What is a notified disease?
- Notified diseases are also called Notifiable diseases. It is any disease whose occurrence has to be reported to the Government by law.
WHO on Notifiable Diseases:
- The WHO International Health Regulations, 1969 has made disease reporting mandatory. This will help WHO in its global surveillance and advisory role. Currently the list is limited only to three main disease namely yellow fever, cholera and plague. And of course COVID-19.
OIE on Notified diseases:
- The OIE, World Organisation for Animal Health monitors diseases of animals at global level. It holds a list of notifiable diseases.
Can Central Government declare notified disease?
- As Health is a State subject, only the State Governments have powers to declare notified diseases. However, the Central Government maintains a list of Notified diseases.
List of Notified Diseases in India:
- AIDS, Hepatitis B, Dengue Fever, Malaria, Whooping cough, Anaemia, Measles, Rabies, Vitamin A deficiency, typhoid, scarlet fever, polio, cerebro spinal fever, leprosy, hepatitis, Cholera, Iodine deficiency, malnutrition, tuberculosis, small pox, plague, measles, influenza, diphtheria, chicken pox.
About Malaria:
- Malaria has been one of the world’s deadliest diseases. It kills more than 400,000 people a year worldwide and causes illness in millions of others.
- Africa is home to 70% of the world’s malaria cases and 90% of deaths.
- In the past two decades, existing interventions have reduced the malaria burden. And India, too, has made good progress in malaria control. The disease burden has declined by 59 per cent.
- The success has led to the government in making a commitment to eliminate malaria by 2030.
- Malaria is caused by Plasmodium; the parasites are spread to people through the bites of infected female Anopheles mosquitoes, called “malaria vectors.”
- There are 5 parasite species that cause malaria in humans, and 2 of these species – falciparum and P. vivax – pose the greatest threat.
- In 2018, falciparum accounted for 99.7% of estimated malaria cases in the WHO African Region 50% of cases in the WHO South-East Asia Region, 71% of cases in the Eastern Mediterranean and 65% in the Western Pacific.
- Vivax is the predominant parasite in the WHO Region of the Americas, representing 75% of malaria cases.
What are the Symptoms?
- Malaria is an acute febrile illness. In a non-immune individual, symptoms usually appear 10–15 days after the infective mosquito bite. The first symptoms – fever, headache, and chills – may be mild and difficult to recognize as malaria. If not treated within 24 hours, falciparum malaria can progress to severe illness, often leading to death.
- Children with severe malaria frequently develop one or more of the following symptoms: severe anaemia, respiratory distress in relation to metabolic acidosis, or cerebral malaria. In adults, multi-organ failure is also frequent. In malaria endemic areas, people may develop partial immunity, allowing asymptomatic infections to occur.
What are its Prevention?
- Vector control is the main way to prevent and reduce malaria transmission. If coverage of vector control interventions within a specific area is high enough, then a measure of protection will be conferred across the community.
- WHO recommends protection for all people at risk of malaria with effective malaria vector control. Two forms of vector control – insecticide-treated mosquito nets and indoor residual spraying – are effective in a wide range of circumstances.
What are the India’s efforts to fight Malaria?
- Indian government has released a National Strategic Plan (NSP) for malaria elimination for years 2017-2022, targeting eradication by 2030.
- This marked a shift in focus from malaria “control” to “elimination”. The plan provides a roadmap to achieve the target of ending malaria in 571 districts out of India’s 678 districts by 2022.
- India has sustained significant decline in malaria cases, halving numbers to 5.1 million in 2018 from 9.6 million the year before. This followed a 24% decline in 2017, according to the World Malaria Report 2018.
- Since 2000, India has reduced malaria deaths by two-thirds and halved the number of malaria cases.Scaling up a diagnostic testing, treatment and surveillance
- Ensuring an uninterrupted drug and diagnostics supply chain. Training community workers to test all fever cases and provide medicines, and distributing medicated bed-nets for prevention, under its ‘test-treat-track’ in the endemic north-eastern states and Odisha.
H3N2 – Influenza
10, Mar 2023

Why in News?
- Across India, an outbreak of a respiratory illness with symptoms of cold, sore throat and fever accompanied by fatigue has been observed since December 2022 and January 2023.
About the News:
- The Indian Council of Medical Research (ICMR) confirmed that Influenza Sub-type H3N2 has been causing this illness.
- It further warned that the virus appeared to lead to more hospitalisations than other Influenza subtypes.
What is H3N2 Virus?
- H3N2 virus is a type of influenza virus called the influenza A virus. It is a respiratory viral infection that causes illnesses every year. This subtype of influenza A virus was discovered in 1968 in humans.
- The virus derives from types of protein strains of the influenza A virus – hemagglutinin (HA) and neuraminidase (NA).
- HA has over 18 different subtypes, each numbered H1 to H18 while NA has 11 different subtypes, each numbered N1 to N11. The H3N2 is a combination of the two protein strains of the influenza A virus.
Symptoms of H3N2 Virus:
- The symptoms of the H3N2 virus include cough, runny nose or congested nose, sore throat, headaches, body aches, fever, chills, fatigue, diarrhoea, vomiting and breathlessness.
Treatment for H3N2 Virus:
- Regular over-the-counter medications for fever, cough or headaches can be consumed to relieve the symptoms.
- Annual flu shots for the influenza virus should be administered and taken around this time.
Types of Influenza Virus:
- There are four types of influenza viruses: influenza A, B, C and D
- Influenza A and B are the two types of influenza that cause epidemic seasonal infections nearly every year.
- Influenza C mainly occurs in humans, but has been known to also occur in dogs and pigs.
- Influenza D is found mainly in cattle. It’s not known to infect or cause illness in humans yet.
H5N1- Avian Influenza
15, Feb 2023

Why in News?
- Recent reports of H5N1 (subtype of avian influenza) being transmitted between mammals have raised concerns about its potential to cause a human pandemic.
About the News:
- Scientists are investigating a potential spillover event after a mass mortality event that killed over 700 seals along the Caspian Sea coast where a H5N1 variant was detected in wild birds a few months ago.
What is H5N1 Avian Influenza?
- Avian influenza or bird flu refers to the disease caused by infection with avian influenza Type A viruses.
- Infrequently, the virus can infect mammals from birds, a phenomenon called spillover, and rarely can spread between mammals.
- H5N1, a subtype of avian influenza, has the potential to infect other mammals such as minks, ferrets, seals, domestic cats, and others through contact with infected birds, their faeces, or infected bird carcasses.
Symptoms in Humans:
- Range from mild to severe influenza-like illnesses such as fever, cough, sore throat, muscle aches, nausea, abdominal pain, diarrhea, vomiting.
- People can also develop severe respiratory illness (e.g., difficulty breathing, pneumonia, acute respiratory distress, viral pneumonia) and altered mental status, seizures etc.
Avian Influenza in India:
- In 2019, India has been declared free from Avian Influenza (H5N1), which has also been notified to the World Organization for Animal Health (OIE).
- However, in December 2020 and early 2021, outbreaks of avian influenza H5N1 and H5N8 were reported in poultry in 15 states in India.
Treatment:
- Evidence suggests that some antiviral drugs can reduce the duration of viral replication and improve prospects of survival, however ongoing clinical studies are needed.
Concerns:
- The widespread H5N1 outbreaks have substantial economic impact, resulting in significant losses to the poultry industry and threatening food and vaccine security, apart from raising animal welfare and environmental concerns.
Types of Influenza Virus:
- There are four types of influenza viruses: influenza A, B, C, and D
- Influenza A and B are the two types of influenza that cause epidemic seasonal infections nearly every year.
- Influenza C mainly occurs in humans, but has been known to also occur in dogs and pigs.
- Influenza D is found mainly in cattle. It’s not known to infect or cause illness in humans yet.
Avian influenza Type A Viruses
- Type A viruses are classified based on two proteins on their surfaces – Hemagglutinin (HA) and Neuraminidase (NA). There are about 18 HA subtypes and 11 NA subtypes.
- Several combinations of these two proteins are possible e.g., H5N1, H7N2, H9N6, H17N10, H18N11 etc.
- All known subtypes of influenza A viruses can infect birds, except subtypes H17N10 and H18N11, which have only been found in bats.
Global Report on Neglected Tropical Diseases
02, Feb 2023
Why in News?
- Recently, the World Health Organization’s (WHO) has released a Global report on Neglected Tropical Diseases (NTD) 2023, which states that NTD continues to disproportionately impact the most impoverished members of the international community.
About the News:
- World NTD day is observed every year on 30th January. It was declared in the 74th World Health Assembly (2021).
What are Neglected Tropical Diseases (NTDs)?
- NTDs are a group of infections that are most common among marginalized communities in the developing regions of Africa, Asia and the Americas.
- They are caused by a variety of pathogens such as viruses, bacteria, protozoa and parasitic worms.
- NTDs are especially common in tropical areas where people do not have access to clean water or safe ways to dispose of human waste.
- These diseases generally receive less funding for research and treatment than malaises like tuberculosis, HIV-AIDS and malaria.
- Examples of NTDs are: snakebite envenomation, scabies, yaws, trachoma, Leishmaniasis and Chagas disease etc.
What are the Highlights of the Report?
- About 16 countries accounted for 80 % of the global NTD burden.
- Globally, nearly 1.65 billion people are estimated to require treatment for at least one NTD.
- Covid-19 impacted the community-based initiatives, access to healthcare facilities and healthcare goods supply chains. As a result, between 2019 and 2020, 34% fewer persons received treatment for NTDs.
Recommendations:
- Greater efforts and investments are required to reverse delays and accelerate progress towards the NTD road map targets by 2030.
- WHO urged multi-sectoral collaboration and partnerships to achieve these targets.
- It is the need of the hour for additional partners and funders to step up and close the gaps preventing the full-scale implementation of NTD actions at the international and local levels.
What are the Global Initiatives?
- WHO’s New Roadmap for 2021–2030: The NTD road map 2021–2030 is WHO’s blueprint to drive global efforts in the fight against NTDs in the context of the United Nations Sustainable Development Goals.
- The Blueprint recommends following measures,
- From measuring process to measuring impact.
- From disease-specific planning and programming to collaborative work across sectors.
- From externally driven agendas reliant to programmes that are country-owned and country-financed.
- London Declaration on NTDs: It was adopted on 30th January, 2012 to recognise the global burden of NTDs.
What are the Indian Initiatives to Eliminate NTDs?
- The Accelerated Plan for Elimination of Lymphatic Filariasis (APELF) was launched in 2018, as part of intensifying efforts towards the elimination of NTDs.
- A WHO-supported regional alliance established by the governments of India, Bangladesh, and Nepal in 2005 to expedite early diagnosis and treatment of the most vulnerable populations and improve disease surveillance and control of sandfly populations (Kala-azar). India has already eliminated several other NTDs, including guinea worm, trachoma, and yaws.
- Preventive methods like Mass Drug Administration (MDA) rounds are periodically deployed in endemic areas during which anti-filarial medicines are provided free-of-cost to at-risk communities.
- Vector-control measures like Indoor Residual Spraying rounds are undertaken in endemic areas to prevent sandfly breeding. The government also supports morbidity management and disability prevention for those affected by lymphoedema and hydrocele.
- State and central governments have also introduced wage compensation schemes for those suffering from Kala-Azar and its sequela (a condition which is the consequence of a previous disease or injury) known as Post-Kala Azar Dermal Leishmaniasis.
India’s Target on Measles and Rubella
25, Jan 2023
Why in News?
- India had set a target to eliminate Measles and Rubella (MR) by 2023, having missed the earlier deadline of 2020, due to a variety of reasons, exacerbated by disruptions due to the pandemic.
About the News:
- In 2019, India adopted the goal of measles and rubella elimination by 2023, anticipating that the 2020 goal could not be reached.
What are Measles and Rubella?
Measles:
- It is a highly contagious viral disease and is a cause of death among young children globally.
- It is caused by a single-stranded, enveloped RNA virus with 1 serotype. It is classified as a member of the genus Morbillivirus in the Paramyxoviridae family.
- It is particularly dangerous for children from the economically weaker background, as it attacks malnourished children and those with reduced immunity.
- It can cause serious complications, including blindness, encephalitis, severe diarrhoea, ear infection and pneumonia.
Rubella:
- It is also called German Measles.
- Rubella is a contagious, generally mild viral infection that occurs most often in children and young adults.
- It is caused by the rubella virus which is an enveloped single-stranded RNA virus.
- Rubella infection in pregnant women may cause death or congenital defects known as Congenital Rubella Syndrome (CRS) which causes irreversible birth defects.
- Rubella isn’t the same as measles, but the two illnesses share some signs and symptoms, such as the red rash.
- Rubella is caused by a different virus than measles, and rubella isn’t as infectious or as severe as measles.
What is the Global and Indian Scenario of Measles and Rubella?
- The measles virus is one of the world’s most contagious human viruses that kills more than 1,00,000 children every year globally, and rubella is a leading vaccine-preventable cause of birth defects, according to the World Health Organization (WHO).
- Over the past two decades, the measles vaccine is estimated to have averted more than 30 million deaths globally, as per the WHO’s statistics.
- During 2010–2013, India conducted a phased measles catch-up immunisation for children aged 9 months–10 years in 14 States, vaccinating approximately 119 million children.
- Mission Indradhanush was launched in 2014 to ramp up vaccinating the unvaccinated population.
- During 2017–2021, India adopted a national strategic plan for measles and rubella elimination.
- During the same period, the Government introduced rubella-containing vaccine (RCV) into the routine immunisation programme.
- As of December 2021, five countries have been verified and have sustained measles elimination – Bhutan, DPR Korea, Maldives, Sri Lanka, Timor-Leste. In addition, Maldives and Sri Lanka have sustained their rubella elimination status in 2021.
What are Measures to Curb MR?
- Measles-Rubella Vaccination: The MR campaign targets around 41 crore children across the country, the largest ever in any campaign.
- All children aged between 9 months and less than 15 years are given a single shot of MR vaccination irrespective of their previous measles/rubella vaccination status or measles/rubella disease status.
- Other Initiatives include Universal Immunization Programme (UIP), Mission Indradhanush and Intensified Mission Indradhanush.
- The vaccines for the diseases are provided in the form of measles-rubella (MR), measles-mumps-rubella (MMR) or measles-mumps-rubella-varicella (MMRV) combination.
Sale of pork banned in the Nilgiris due to African Swine Fever outbreak
09, Jan 2023

Why in News?
- The sale of pork in the Nilgiris and the transportation of animals or meat outside the Nilgiris has been banned following an outbreak of African Swine Fever (ASF) among wild boar populations in Mudumalai and Bandipur Tiger Reserves.
About the infection:
- It is a highly contagious and fatal animal disease that infects and leads to an acute form of haemorrhagic fever in domestic and wild pigs.
- Other manifestations of the disease include high fever, depression, anorexia, loss of appetite, haemorrhages in the skin, vomiting and diarrhoea among others.
- It was first detected in Africa in the 1920s.
- Historically, outbreaks have been reported in Africa and parts of Europe, South America, and the Caribbean.
- However, more recently (since 2007), the disease has been reported in multiple countries across Africa, Asia and Europe, in both domestic and wild pigs.
- The mortality is close to 100% and since the fever has no cure, the only way to stop its spread is by culling the animals.
- ASF is not a threat to human beings since it only spreads from animals to other animals.
- ASF is a disease listed in the World Organisation for Animal Health (OIE) Terrestrial Animal Health Code and thus, reported to the OIE.
What is Classical Swine Fever?
- CSF, also known as hog cholera, is an important disease of pigs.
- It is one of the most economically-damaging pandemic viral diseases of pigs in the world.
- It is caused by a virus of the genus Pest virus of the family Flaviviridae, which is closely related to the viruses that cause bovine viral diarrhoea in cattle and border disease in sheep.
- Mortality is 100%.
- Recently, the ICAR-IVRI developed a Cell Culture CSF Vaccine (live attenuated) using the Lapinized Vaccine Virus from foreign strain.
- The new vaccine has been found to induce protective immunity from day 14 of the Vaccination till 18 Months.
About World Organisation for Animal Health:
- OIE is an intergovernmental organisation responsible for improving animal health worldwide.
- It has 182 Member Countries. India is one of the member countries.
- OIE develops normative documents relating to rules that Member Countries can use to protect themselves from the introduction of diseases and pathogens. One of them is the Terrestrial Animal Health Code.
- OIE standards are recognised by the World Trade Organization as reference international sanitary rules.
- It is headquartered in Paris, France.
Antimicrobial Resistance
12, Dec 2022
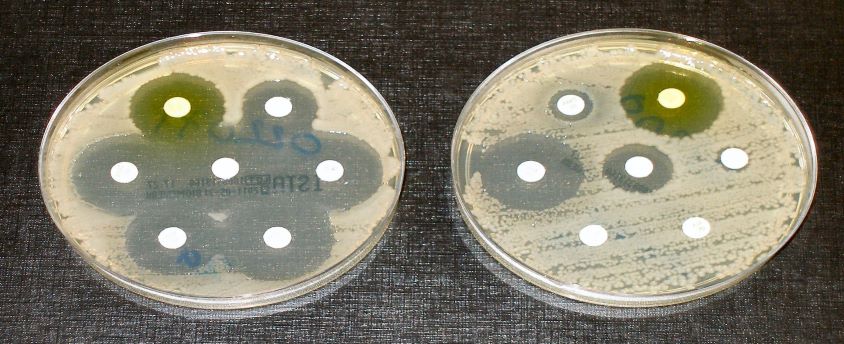
Why in News?
- Over 50% of life-threatening bacterial infections are becoming resistant to treatment: the Global Antimicrobial Resistance and Use Surveillance System (GLASS) report of WHO.
What are the concerns as per the recent report?
- 8% of infections caused by Klebsiella pneumonia were resistant to carbapenems (the last resort antibiotic).
- Over 60% of Neisseria gonorrhoea, a common sexually transmitted disease, show resistance to ciprofloxacin.
- 20% of coli isolates, common in urinary tract infections were resistant to ampicillin and co-trimoxazole.
- Bloodstream infections due to resistant coli, Salmonella and gonorrhoea infections, have jumped by at least 15 per cent compared to 2017 rates.
About Global Antimicrobial Resistance and Use Surveillance System (GLASS):
- Provides a standardized approach to the collection, analysis, interpretation and sharing of data by countries and seeks to actively support capacity building and monitor the status of existing and new national surveillance systems.
What is AMR?
- Antimicrobial resistance is the resistance acquired by any microorganism (bacteria, viruses, fungi, parasite, etc.) against antimicrobial drugs (such as antibiotics, antifungals, antivirals, antimalarials, and anthelmintics) that are used to treat infections.
- As a result, standard treatments become ineffective, infections persist and may spread to others.
- Microorganisms that develop antimicrobial resistance are sometimes referred to as “superbugs”.
- The World Health Organization (WHO) has identified AMR as one of the top ten threats to global health.
Reasons for Spread of AMR:
- The misuse of antimicrobials in medicine and inappropriate use in agriculture.
- Contamination around pharmaceutical manufacturing sites where untreated waste releases large amounts of active antimicrobials into the environment.
What Initiatives have been taken by the Government to Prevent AMR?
- AMR Surveillance and Research Network (AMRSN) was launched in 2013, to generate evidence and capture trends and patterns of drug resistant infections in the country.
- The National Action Plan on AMR focuses on One Health approach and was launched in April 2017 with the aim of involving various stakeholder ministries/departments.
- ICMR along with Research Council of Norway (RCN) initiated a joint call for research in antimicrobial resistance in 2017.
- ICMR along with the Federal Ministry of Education and Research (BMBF), Germany has a joint Indo-German collaboration for research on AMR.
- ICMR has initiated Antibiotic Stewardship Program (AMSP) on a pilot project across India to control misuse and overuse of antibiotics in hospital wards and ICUs.
Recommendation by WHO:
- Equitable and global access to the vaccines that already exist
- Disruptive approaches are needed: The lessons from COVID 19 vaccine development and mRNA vaccines offer unique opportunities to explore for development of vaccines against bacteria
- Need to overcome challenges: Such as pathogens associated with hospital-acquired infections (HAI), difficulty in defining target population(s) among all admitted hospital patients; the cost and complexity of vaccine efficacy trials; and the lack of regulatory and/or policy precedent for vaccines against HAIs.
- Easier regulatory requirement: Vaccine development is expensive, and scientifically challenging, and is associated with high failure rates, and therefore, the need for support from the government and private sector.
Antimicrobial Resistance Vaccines
03, Dec 2022

Why in News?
- Antimicrobial resistance (AMR) has been declared one of the top global public health threats by the World Health Organization (WHO).
Background:
- In 2019, an overall 95 million deaths were caused by AMR infections and associated complications.
- India is the world’s largest consumer of antibiotics and has the world’s highest infectious disease burden including due to multi-resistant pathogens (superbugs).
- AMR may cause a global annual GDP loss of $3.4 trillion by 2030 and may push 24 million people into extreme poverty.
What is AMR?
- Antimicrobial resistance is the resistance acquired by any microorganism (bacteria, viruses, fungi, parasite, etc.) against antimicrobial drugs (such as antibiotics, antifungals, antivirals, antimalarials, and anthelmintics) that are used to treat infections.
- As a result, standard treatments become ineffective, infections persist and may spread to others.
- Microorganisms that develop antimicrobial resistance are sometimes referred to as “superbugs”.
- The World Health Organization (WHO) has identified AMR as one of the top ten threats to global health.
Reasons for Spread of AMR:
- The misuse of antimicrobials in medicine and inappropriate use in agriculture.
- Contamination around pharmaceutical manufacturing sites where untreated waste releases large amounts of active antimicrobials into the environment.
What Initiatives have been taken by the Government to Prevent AMR?
- AMR Surveillance and Research Network (AMRSN) was launched in 2013, to generate evidence and capture trends and patterns of drug resistant infections in the country.
- The National Action Plan on AMR focuses on One Health approach and was launched in April 2017 with the aim of involving various stakeholder ministries/departments.
- ICMR along with Research Council of Norway (RCN) initiated a joint call for research in antimicrobial resistance in 2017.
- ICMR along with the Federal Ministry of Education and Research (BMBF), Germany has a joint Indo-German collaboration for research on AMR.
- ICMR has initiated Antibiotic Stewardship Program (AMSP) on a pilot project across India to control misuse and overuse of antibiotics in hospital wards and ICUs.
Recommendation by WHO:
- Equitable and global access to the vaccines that already exist
- Disruptive approaches are needed: The lessons from COVID 19 vaccine development and mRNA vaccines offer unique opportunities to explore for development of vaccines against bacteria
- Need to overcome challenges: Such as pathogens associated with hospital-acquired infections (HAI), difficulty in defining target population(s) among all admitted hospital patients; the cost and complexity of vaccine efficacy trials; and the lack of regulatory and/or policy precedent for vaccines against HAIs.
- Easier regulatory requirement: Vaccine development is expensive, and scientifically challenging, and is associated with high failure rates, and therefore, the need for support from the government and private sector.
Antimicrobial Resistance Vaccines
19, Nov 2022
Why in News?
- Poor animal health in factory farming can negatively affect food safety, our environment and climate, leading to Antimicrobial Resistance (AMR).
What are the Issues?
- Factory farming or intensive food-animal farming is the intense and confined farming of animals such as pigs, cows, and birds. They are industrial facilities that raise large numbers of animals, mostly indoors, in conditions intended to maximise production at a minimal cost.
- The suffering of animals within farms around the world is too often overlooked or seen to be separate from the big issues such as pandemics and the public health crisis, climate change and biodiversity loss, food insecurity and malnutrition.
- In reality, this can exacerbate the global problems as well as causing immense cruelty to billions of animals.
- Producing more than 50 billion factory-farmed land animals each year to satisfy growing demand for cheap meat requires using breeds of genetically uniform animals squashed together, creating an ideal breeding ground for disease that can jump to humans.
- When diseases jump from one species to another, they often become more infectious and cause more serious illness and death, leading to global pandemics.
- Bird flu and swine flu are two key examples where new strains constantly emerge from intensively farmed animals.
- However, there is an addition to this list — Antimicrobial Resistance which is overlooked among these big issues.
- The overuse of antibiotics on factory farms leads to superbugs that spread to workers, the environment and into the food chain.
- Factory farms, characterised by substandard husbandry practices and poor animal welfare, drive the increased use of antimicrobials, and are connected to the emergence of AMR alongside a range of zoonotic pathogens.
What is AMR?
- Antimicrobial resistance is the resistance acquired by any microorganism (bacteria, viruses, fungi, parasite, etc.) against antimicrobial drugs (such as antibiotics, antifungals, antivirals, antimalarials, and anthelmintics) that are used to treat infections.
- As a result, standard treatments become ineffective, infections persist and may spread to others.
- Microorganisms that develop antimicrobial resistance are sometimes referred to as “superbugs”.
- The World Health Organization (WHO) has identified AMR as one of the top ten threats to global health.
Reasons for Spread of AMR:
- The misuse of antimicrobials in medicine and inappropriate use in agriculture.
- Contamination around pharmaceutical manufacturing sites where untreated waste releases large amounts of active antimicrobials into the environment.
What Initiatives have been taken by the Government to Prevent AMR?
- AMR Surveillance and Research Network (AMRSN) was launched in 2013, to generate evidence and capture trends and patterns of drug resistant infections in the country.
- The National Action Plan on AMR focuses on One Health approach and was launched in April 2017 with the aim of involving various stakeholder ministries/departments.
- ICMR along with Research Council of Norway (RCN) initiated a joint call for research in antimicrobial resistance in 2017.
- ICMR along with the Federal Ministry of Education and Research (BMBF), Germany has a joint Indo-German collaboration for research on AMR.
- ICMR has initiated Antibiotic Stewardship Program (AMSP) on a pilot project across India to control misuse and overuse of antibiotics in hospital wards and ICUs.
Recommendation by WHO:
- Equitable and global access to the vaccines that already exist
- Disruptive approaches are needed: The lessons from COVID 19 vaccine development and mRNA vaccines offer unique opportunities to explore for development of vaccines against bacteria
- Need to overcome challenges: Such as pathogens associated with hospital-acquired infections (HAI), difficulty in defining target population(s) among all admitted hospital patients; the cost and complexity of vaccine efficacy trials; and the lack of regulatory and/or policy precedent for vaccines against HAIs.
- Easier regulatory requirement: Vaccine development is expensive, and scientifically challenging, and is associated with high failure rates, and therefore, the need for support from the government and private sector.
WHO Emergency Nod for Serum Institute’s Covovax
28, Dec 2021
Why in News?
- The WHO recently issued an emergency use listing (EUL) for NVX-CoV2373, or Covovax, the anti-Covid vaccine being produced by the Pune-based Serum Institute of India (SII) under Licence from Novavax.
About the News:
- Covovax is the first protein-based Covid-19 vaccine option with demonstrated efficacy and a well-tolerated safety profile to be made available through the COVAX Facility.
- Covovax is a subunit of the vaccine developed by Novavax and the Coalition for Epidemic Preparedness Innovations (CEPI). It requires two doses and is stable at 2 to 8°C Refrigerated Temperatures.
- The vaccine uses a novel platform and is produced by creating an engineered baculovirus Containing a gene for a modified SARS-CoV-2 spike protein.
What is the Regular Procedure for Drug Approval?
- Vaccines and medicines, and even diagnostic tests and medical devices, require the approval of a regulatory authority before they can be administered.
- In India, the regulatory authority is the Central Drugs Standard Control Organisation (CDSCO).
- For vaccines and medicines, approval is granted after an assessment of their safety and effectiveness, based on data from trials.
About CDSCO:
- The Central Drugs Standard Control Organisation (CDSCO) under Directorate General of Health Services, Ministry of Health & Family Welfare, Government of India is the National Regulatory Authority (NRA) of India.
- Under the Drugs and Cosmetics Act, CDSCO is responsible for
- Approval of New Drugs
- Conduct of Clinical Trials
- Laying down the standards for Drugs
- Control over the quality of imported Drugs in the country and
- Coordination of the activities of State Drug Control Organizations by providing expert advice with a view to bring about the uniformity in the enforcement of the Drugs and Cosmetics Act.
- CDSCO along with state regulators is jointly responsible for grant of licenses of certain specialized categories of critical Drugs such as blood and blood products, Vaccine and Sera.
When can Emergency use Authorisation (EUA) be granted?
- In the US, the Food and Drug Administration (FDA) grants EUA only after it has been determined that the “known and potential benefits outweigh the known and potential risks of the vaccine” (or medicine).
- This means that a EUA application can be considered only after sufficient efficacy data from phase 3 trials had been generated.
- A EUA cannot be granted solely on the basis of data from phase 1 or phase 2 trials.
What is the process of Getting an Emergency use Authorisation in India?
- Experts and activists say India’s drug regulations do not have provisions for a EUA, and the process for receiving one is not clearly defined or consistent.
- Previously it has been granted permission for Covaxin and Covishield and covaxin emerged as the first COVID-19 vaccine globally to be used for vaccinating children as young as 2 years.
About WHO’s Emergency Use List (EUL):
- The WHO Emergency Use Listing Procedure (EUL) is a risk-based procedure for assessing and listing unlicensed vaccines, therapeutics and in vitro diagnostics with the ultimate aim of expediting the availability of these products to people affected by a public health emergency.
- To be eligible, the following criteria must be met:
- The disease for which the product is intended is serious or immediately life threatening, has the potential of causing an outbreak, epidemic or pandemic and it is reasonable to consider the product for an EUL assessment, e.g., there are no licensed products for the indication or for a critical subpopulation (e.g., children).
- Existing products have not been successful in eradicating the disease or preventing outbreaks (in the case of vaccines and medicines).
- The product is manufactured in compliance with current Good Manufacturing Practices (GMP) in the case of medicines and vaccines and under a functional Quality Management System (QMS) in the case of IVDs.
- The applicant undertakes to complete the development of the product (validation and verification of the product in the case of IVDs) and apply for WHO prequalification once the product is licensed.
USE OF TB DRUGS ON CROPS
12, May 2020

Why in News?
- Registration Committee (RC) under the Central Insecticides Board and Registration Committee (CIBRC) has recently recommended to ban the use of antibiotics streptomycin and tetracycline for Bacterial Disease Control in Plant crops.
Key Points:
- The RC Recommended to ban Antibiotics Streptomycin and Tetracycline with Immediate effect on crops where other options are available for bacterial disease control.
- Where no alternatives are available, use of these antibiotics should be phased out by 2022-end. Till then, the Antibiotics could be used on crops strictly as per the Label claim i.e. streptomycin sulphate (9%) and tetracycline hydrochloride (1%).
- The RC acknowledged that diseases in crops can be managed by using Integrated pest management and other practices.
Issues Involved:
- Rampant Misuse: Although Streptocycline use is Allowed for eight crops by the CIBRC, it was found to be used on Many More Crops in practice.
- Antibiotic Resistance:Exposure to antibiotics can lead to Development of antibiotic resistance in Humans and Animals.
What is Streptomycin?
- It is also used in multidrug-resistant TB patients and in certain cases of TB meningitis (brain TB).It has important use for previously treated tuberculosis (TB) patients.6
- The World Health Organization (WHO) recognises streptomycin as a critically important medicine for human use.
About Central Insecticides Board & Registration Committee:
- The Central Insecticides Board & Registration Committee (CIBRC) was set up by the Ministry of Agriculture and Farmers Welfare in the year 1970 to regulate the import, manufacture, sale, transport, distribution and use of insecticides.
- The Insecticides are Regulated under Insecticides Act, 1968 and Insecticides Rules, 1971.
- The Central Insecticides Board (CIB) advises the Central Government and State Governments on technical matters arising out of the administration of Insecticides Act and to carry out the other functions assigned to the Board by or under Insecticides rules.
- To import or Manufacture any Insecticide, Registration is required at the Registration Committee.
SAFEGUARDS AGAINST CHEMICAL DISASTERS IN INDIA
09, May 2020

Why in News?
- Vizag gas leak tragedy has put the spotlight on the safeguards available against chemical disasters in India.
Law before Bhopal Gas Tragedy:
- At the time of the Bhopal gas tragedy, the Indian Penal Code (IPC) was the only relevant law specifying criminal liability for such Incidents.
- Section 304: culpable homicide not amounting to murder.
- Section 304A: deals with death due to negligence and imposes a maximum punishment of two years and a fine.
- Soon after the tragedy, the government passed a series of laws regulating the environment and prescribing and specifying safeguards and penalties.
Laws after Bhopal Gas Tragedy:
- Bhopal Gas Leak (Processing of Claims) Act, 1985, which gives powers to the central government to secure the claims arising out of or connected with the Bhopal gas tragedy. Under the provisions of this Act, such claims are dealt with speedily and equitably.
- The Environment Protection Act, 1986, which gives powers to the central government to undertake measures for improving the environment and set standards and inspect Industrial Units.
- Hazardous Waste (Management Handling and Trans boundary Movement) Rules, 1989: Industry required to identify major accident hazards, take preventive measures and submit a report to the Designated authorities.
- Manufacture, Storage and Import of Hazardous Chemicals Rules, 1989: Importer must furnish complete product safety information to the competent authority and must transport imported chemicals in accordance with the amended rules.
- Chemical Accidents (Emergency, Planning, Preparedness and Response) Rules, 1996: Centre is required to constitute a central crisis group for management of chemical accidents; set up quick response mechanism termed as the crisis alert system. Each state is required to set up a crisis group and report on its work.
- The Public Liability Insurance Act, 1991, which is insurance meant to provide relief to persons affected by accidents that occur while handling hazardous substances.
- The National Environment Appellate Authority Act, 1997, under which the National Environment Appellate Authority can hear appeals regarding the restriction of areas in which any industries, operations or processes or class of industries, operations or processes shall not be carried out or shall be carried out subject to certain safeguards under the Environment (Protection) Act, 1986.
- National Green Tribunal, 2010, provides for the establishment of a National Green Tribunal for effective and expeditious disposal of cases related to environmental protection and conservation of forests.
Recent Major Gas-Leak related Disasters:
- 2014 GAIL Pipeline Blast:On 27 June 2014, a massive fire broke out following a blast in the underground gas pipeline maintained by the Gas Authority of India Limited (GAIL) at Nagaram, East Godavari district of Andhra Pradesh.
- 2014 Bhilai Steel Plant Gas Leak: In another incident in June 2014 at Bhilai Steel Plant in Chhattisgarh’s Durg district, six people were killed and over 40 injured in an incident of leakage in a methane gas pipeline at a water pump house.
- 2017 Delhi Gas leak:Around 470 schoolchildren were hospitalised after inhaling poisonous fumes that spread due to a chemical leak at a container depot near two schools in the customs area of Tughlaqabad depot.
- 2018 Bhilai Steel Plant Blast:Nine people were killed and 14 others injured in a blast at the Bhilai Steel Plant of state-owned SAIL.
Cause for Concern Now:
- According to the National Disaster Management Authority (NDMA), in the recent past, over 130 significant chemical accidents have been reported in the country, which have resulted in 259 deaths and caused major injuries to more than 560 people.
- There are over 1861 Major Accident Hazard (MAH) units spread across 301 districts and 25 states and three Union Territories in all zones of the country.
- Further, there are thousands of registered and hazardous factories and un-organised sectors dealing with numerous ranges of hazardous material posing serious and complex levels of Disaster Risks.
STYRENE GAS LEAK IN VIZAK
08, May 2020

Why in News?
- A Gas Leak, Reminiscent of the 1984 Bhopal tragedy, has affected thousands of residents in five villages in Visakhapatnam in Andhra Pradesh.
About the News:
- The source of the leak was a styrene plant owned by South Korean electronics giant LG, located at RRV Puram near Gopalapatnam, about 15 kms from the coast city.
- A statement from LG Polymers said that stagnation and changes in temperature inside the storage tank could have resulted in auto polymerization and could have caused vapourisation.
What is Styrene?
- It is a flammable liquid that is used in the manufacturing of polystyrene plastics, fiberglass, rubber, and latex.
- It is also found in vehicle exhaust, cigarette smoke, and in natural foods like fruits and vegetables.
What happens when Exposed to Styrene?
- Short-term exposure to the substance can result in respiratory problems, irritation in the eyes, irritation in the mucous membrane, and gastrointestinal issues.
- Long-term exposure could drastically affect the central nervous system and lead to other related problems like peripheral neuropathy. It could also lead to cancer and depression in some cases.
What are the Symptoms?
- Symptoms include headache, hearing loss, fatigue, weakness, difficulty in concentrating etc.
- Animal studies, according to the EPA, have Reported effects on the CNS, Liver, Kidney, and Eye and Nasal Irritation from Inhalation Exposure to styrene.
Other Similar Gas Tragedy in India:
- Bhopal Gas tragedy occurred on the cold wintry night in the early hours of 3 December, 1984.
- At around midnight, the chemical reaction started in the Union Carbide (India) Limited factory that culminated in the leakage of deadly Methyl Isocyanate (MIC) gas from one of the tanks of the factory.
- As a result, a cloud of gas gradually started descending and enveloping the city in its lethal folds. And the city and lakes turned into a gas chamber.
- In the tragedy around 3000 lives of innocent people were lost and thousands and thousands of people were physically impaired or affected in several forms.
- After the tragedy, the government of India enacted a Public Liability Insurance Act (1991), making it mandatory for industries to get insurance the premium for this insurance would contribute to an Environment Relief Fundto provide compensation to victims of a Bhopal-like disaster.
What does PLI Act Say?
- The Public Liability Insurance (PLI) Act, 1991 makes it obligatory upon the user industries handling 179 types of chemicals and compounds and other classes of flammable substances to subscribe a special insurance policy to cover the liabilities likely to arise on account of any chemical (industrial) disaster/accident and payable to those affected people who are not the workers on ‘no fault basis’/ ‘absolute liability’.
- The Act establishes an Environment Relief Fund (ERF),which is subscribed by all such user industries by an amount equal to the annual premium amount of such insurance policies.
- PLI Act is administered by the Ministry of Environment Forest and Climate Change.
SILENT OR HAPPY HYPOXIA
07, May 2020
Context:
- Recently, medical practitioners have reported a condition called silent or happy hypoxia, in which patients have extremely low blood oxygen levels, yet they do not show signs of Breathlessness.
- Many of them are now advocating for its early detection as a means to avoid a fatal illness called Covid Pneumonia.
About Hypoxia:
- It is a condition wherein there is not enough oxygen available to the blood and body tissues.
- It can either be Generalised, affecting the whole body, or local, affecting a region of the body.
- The Normal arterial oxygen is approximately 75 to 100 Millimetres of mercury (mm Hg) and normal pulse oximeter readings usually range from 95 to 100%.
- When levels fall below 90%, patients could begin experiencing lethargy, confusion or mental disruptions because of insufficient quantities of oxygen Reaching the Brain.
- When Levels below 80% can result in damage to Vital Organs.
About Silent Hypoxia:
- It is a form of oxygen deprivation that is harder to detect than regular hypoxis because patients appear to be less in distress.
- Covid pneumonia is a serious medical condition found in severe Covid-19 patients, is preceded by silent hypoxia.
- There are many Covid-19 patients with oxygen levels below 80% look at ease and alert. There have been a few cases of oxygen levels below 50% as well.
- Those with such low levels of oxygen would normally appear extremely ill but not in silent Hypoxia Cases.
- Covid-19 Patients with Silent Hypoxia did not Exhibit Symptoms such as shortness of breath or coughing until their oxygen fell to acutely low levels, at which point there was a risk of acute respiratory distress (ARDS) and organ failure.
- Reason why people are left feeling breathless
- It is not because of the fall in oxygen levels itself but due to the rise in carbon dioxide levels that occur at the same time, when lungs are not able to expel this gas efficiently.
- In some Covid-19 cases, this was not the response and patients did not feel breathless.
- It happened because in patients with Covid pneumonia, the virus causes air sacs to fall, leading to a reduction in levels of oxygen.
- However, the lungs initially do not become stiff or heavy with fluid and remain compliant meaning they are able to expel carbon dioxide and avoid its buildup. Thus, patients do not feel short of breath.
- A medical device called a pulse oximeter can be used in the early detection of silent hypoxia.
About Pulse Oximeter:
- It is a test used to measure the oxygen level (oxygen saturation) of the blood.
- It measures the saturation of oxygen in red blood cells (RBCs) and can be attached to a person’s fingers, toes, nose, feet, ears or forehead.
- It is easy and painless and the device can be reused or disposed of after use.
- It is generally used to check the health of patients with known conditions that affect blood oxygen levels like heart and lung conditions.
About Covid Pneumonia:
- It is a potentially deadly condition in Covid-19 patients which affects the lungs’ ability to transfer oxygen and causes breathing difficulties.
- When a person cannot inhale enough oxygen and exhale enough carbon dioxide, the pneumonia can lead to death.
- It is especially severe because it is viral and it completely affects the lungs instead of small parts.
- The Patients are required to be put on ventilator support in such severe cases to ensure adequate circulation of oxygen in the body.
BLOOD CLOTS CAUSED BY CORONAVIRUS
06, May 2020
Why in News?
- The doctors around the world have recently noticed a raft of clotting-related disorders in Covid-19 patients, which causes benign Skin lesions on the feet to strokes and Blood-Vessel Blockages.
Highlights:
- Generally, it was considered that the vast majority of lung damage in Covid-19 patients was due to viral pneumonia.
- But the autopsies of the Covid-19 patients show that clumps of platelets inside blood vessels, or micro thrombi, to be the reason for rapid and dramatic deterioration of condition of patients.
- These blood clots are called thrombi, that form in patients’ arterialcatheters and filters used to support failing kidneys.
- The clots impede blood flow in the lungs, which develop severe blood-oxygen deficiency, causing difficulty in breathing.
- Studies found that as many as 30% of severely ill Covid-19 patients suffered a so-called pulmonaryembolism, a potentially deadly blockage in one of the arteries of the lungs.
- Pulmonary embolism: It often occurs when bits of blood clots from veins deep in the legs travel to the lungs. It was 1.3% in critically ill patients without Covid-19.
- The D-dimer bloodtest is being used around the world to monitor clot formation in patients, including those with Covid-19, and patients are also being dosened with heparin and other anticoagulant medications.
Background of Blood Clotting Diseases:
- In 1918 Spanish flu pandemic, caused by a novel strain of influenza, was also linked to downstream damage from clots that could end lives dramatically.
- The Viruses including HIV, dengue and Ebola are all known to make blood cells prone to clumping.
- The pro-clotting effect may be even more pronounced in patients with the coronavirus.
Issues of Blood Clotting’s in Covid-19 Patients:
- If untreated, Large Arterial lung clots can put overwhelming strain on the heart, causing cardiac arrest. Even tiny clots in the capillaries of lung tissue may interrupt blood flow, undermining attempts to help oxygenate patients with ventilators.
- These Clots may form in other parts of the body, potentially damaging vital organs including the heart, kidneys, liver, bowel, and other tissues.
- The Covid-19 survivors who have subsequent difficulty breathing, might mistakenly believe it’s a recurrence of coronavirus infection, when it may actually be a reactivation of the whole clotting problem.
- The Pulmonary embolism also causes Pulmonary Hypertension, Another Dangerous complication that can cause fatigue and shortness of breath.
- Risk: Patients and doctors alike may not be aware of the risks or the Potential need for Treatment.
WHO RAISES CONCERN OVER USE OF BCG VACCINE
02, May 2020
Why in News?
- World Health Organization (WHO) Director-General Tedros A Ghebreyesus and others highlight a few critical issues over the use of BCG vaccine for COVID-19.
About BCG:
- Bacillus Calmette–Guerin (BCG) vaccine is a vaccine primarily used against tuberculosis (TB). In countries where TB or leprosy is common, one dose is recommended in healthy babies as close to the time of birth as possible.
- In areas where tuberculosis is not common, only children at high risk are typically immunized, while suspected cases of tuberculosis are individually tested for and treated.
BCG and COVID-19:
- The Middle and High-Income Countries
- Countries that have universal BCG policy had 0.78 deaths per million people.
- The countries that never had a universal BCG policy had a larger mortality rate, with 16.39 deaths per million people, a significant variation.
- Low and Middle-Income Countries, even if they had universal immunisation policies, were excluded from the analysis because they were also likely to have low testing rates for COVID-19 infection and therefore fewer reported deaths.
- India having a universal BCG policy in place and relatively fewer deaths as a proportion of confirmed coronavirus infections, wasn’t included in the analysis.
- The BCG vaccine is known to confer a strong immune response and a significant degree of protection against leprosy and non-invasive bladder cancers.
- Those countries where the elderly was likely to have had a BCG shot in their childhood were likely to be better protected against coronavirus because COVID-19 was particularly lethal to the Elderly.
BCG in Cases of Different Countries:
- Japan (which has a BCG policy since 1947) had one of the early cases of COVID-19 but it has maintained a low mortality rate despite not implementing the most strict forms of social isolation.
- Japan had 1,655 cases and 65 deaths as of March 29.
- Iran, which has seen at least 3,000 deaths, began implementing its BCG vaccination policy only in 1984 and therefore anyone over 36 was vulnerable.
- Spain, France, the United States, Italy and the Netherlands:
- These countries don’t have universal BCG policies and have seen many deaths from COVID-19.
- Many of these countries don’t have a universal programme because BCG has been shown to not be always protective against tuberculosis in adults as well as an increased risk of mycobacterium (bacteria) species.
- Italy, where the COVID-19 mortality is very high, never implemented universal BCG vaccination.
What are the Concerns of WHO?
- The authors cite five reasons countries should wait for the results of the BCG vaccine Randomised controlled trials.
- According to them, the association of fewer COVID-19 cases in countries that have a universal BCG Vaccination Programme is based on population rather than individual data.
- Second, the beneficial effects of the BCG vaccine given at birth are “unlikely” to reduce the severity of COVID-19 decades later. “One reason for this is that the beneficial off-target effects of the BCG vaccine might be altered by subsequent administration of a different vaccine.
- Third, there is a possibility, even if remote, that the BCG vaccine ramps up the immune system leading to exacerbation of COVID-19 in a small population of patients with a severe disease.It is already known that the virus induces cytokine storm in some patients, leading to further complications — and even death.
- Fourth, if not effective against the novel coronavirus, BCG vaccination is likely to give a false sense of security to people, especially during the pandemic.
- And finally, using the vaccine without evidence of its benefits could further Jeopardise vaccine supply, which is already short, to protect children against disseminated TB in high-risk Countries.
HUMAN CHALLENGE TRIALS
30, Apr 2020
Why in News:
- Recently, many people have volunteered to take part in the Human Challenge Trials (HCTs). It involves intentionally infecting volunteers with the novel coronavirus, in order to speed up the vaccination development.
About the Vaccine Development:
- Generally, vaccines take several years to develop and their development typically proceeds through three phases of clinical trials.
- In Phase 1, a Small Groups of People receive the Trial Vaccine.
- In Phase 2, the Clinical study is expanded and the vaccine is given to people who have characteristics (such as age and physical health) similar to those for whom the new vaccine is intended.
- In Phase 3, the Vaccine is given to several thousand people and tested for efficacy and safety. During this phase, participants either receive the vaccine or a placebo.
- Its efficacy is determined by comparing the prevalence of infection in the group that was administered the vaccine with the one which received a placebo.
- Placebo is anything which looks like real treatment but it is actually not. For example- sugar pills and saline injections.
What is Human Challenge Trials?
- It means the participants of both the vaccine group and placebo group are deliberately exposed to the infection after their consent and thus are challenged by the disease organism.
- It is not new and they are usually carried out in developing medications for diseases which are considered less lethal and have been better understood by scientists over the years like malaria.
- The scientists have suggested replacing the conventional Phase 3 testing of vaccines by controlled HCTs of Covid-19 (SARS-CoV-2) vaccine which can accelerate the testing and potential rollout of efficacious vaccines.
- It may reduce many months from the licensure process, making efficacious vaccines available more quickly and will also require significantly less number of people than regular Phase 3 trials.
About the Ethical Concerns of Human Trails:
- The trails for Covid-19 have been questioned by critics because it is a potentially deadly disease for even those who are less at risk, and has not been studied fully yet.
- The World Health Organisation (WHO) emphasised on the ethical framework of the challenge studies and also highlighted the importance of informed consent.
- Human challenge studies should be conducted with abundant forethought, caution, and oversight. The value of the information to be gained should clearly justify the risks to Human subjects.
ICMR ASKS STATES TO STOP USING RAPID TESTS
22, Apr 2020

Why in News?
- The Indian Council of Medical Research (ICMR) has directed the States not to use the COVID-19 rapid testing kits for the next two days following reports of wide variations in results.
What is the Issue?
- The Rajasthan government decided to halt rapid antibody tests after an experts’ team questioned the use of the newly distributed Chinese testing kits following inaccurate results.
- The health authorities had started the testing on those with symptoms at designated points recently.
- The quality issues with the test kits, currently being used to study community transmission, would put on hold survey in several States temporarily.
- The kits would be tested and validated by ICMR teams and an advisory on their use issued in the next two days.
- If they were found to be not up to the mark, replacements would be sought from the manufacturers.
What is Rapid Test?
- A rapid test is conducted to determine whether there has been any kind of recent viral infection in a person’s body.
- When a pathogen enters a human body, specific antibodies are released as a response to the virus.
- A rapid test can detect the presence of such antibodies in blood, serum or plasma samples quickly, indicating a viral infection.
- Rapid testing is conducted usually to check for community transmission of a virus during an epidemic.
- Rapid tests can be used to conduct screening within the community and identify those with suspected infection, put them under observation and if required, subject them to the PCR test for coronavirus confirmation.
- According to the health department, it is a simple test that can be done with a person’s blood sample and will give out results within 10-30 minutes. It is also a low-cost test.
Way Forward:
- This has seriously hampered our efforts to get fast test results for starting the treatment and contain the spread of the virus.
- The advisory issued by the ICMR to the States to not use testing kits for the next two days was most unfortunate, as the medical apex body could not ensure good quality of testing kits.
- Even at this late stage, the Centre should take an urgent action to procure the equipment from reliable sources and supply them to the States to get the faster results and start the treatment for the affected.
AAROGYA SETU APP MUST FOR LABOURERS, SAYS CPWD
21, Apr 2020

Why in News?
- Central government organisations involved in construction, were instructed by the Central Public Works Department (CPWD) to ensure that “all labour personnel/staff” returning to work have downloaded the government’s COVID-19 tracking app — Aarogya Setu.
About Aarogya Setu:
- Aarogya Setu app has been launched by the Ministry of Electronics and Information Technology.
- It will help people in identifying the risk of getting affected by the Coronavirus.
- It will calculate risk based on the user’s interaction with others, using cutting edge Bluetooth technology, algorithms and artificial intelligence.
- Once installed in a smartphone, the app detects other nearby devices with Aarogya Setu installed.
- The App will help the Government take necessary timely steps for assessing risk of spread of COVID-19 infection, and ensuring isolation where required.
Why CPWD Initiates such Measure?
- The advisory comes as the Union Home Affairs Ministry has relaxed some restrictions, including for construction activity under certain conditions.
- When the app is installed in a Smartphone it will detect other devices with Aarogya Setu installed that come in proximity of that phone. The app currently supports 11 languages, including Hindi and English.
- After submitting the details, it will cross-checks the detail present in the government database and uses the proximity of Bluetooth and suggests whether the labourer is safe or not.
- In case if a labourer is not safe then the app will suggest to isolate and take precautions.
- The app will also check the user’s location of around six feet that is whether he or she was in the proximity of an infected patient by using the device Bluetooth.
- The app will show that you are at a ‘high risk’ or not. In case you are at a high-risk area then the app advises you to go for a test and call the toll-free number 1075 to schedule an appointment at the nearby testing centre.
About CPWD:
- CPWD came into existence in July, 1854 when Lord Dalhousie established a central agency for execution of public works and set up Ajmer Provincial Division. It is housed under the Ministry of Urban Development.
- Through the professional expertise in disciplines including Architecture, Engineering, Project Management coupled with comprehensive experience in building construction and maintenance, CPWD has been serving the nation for last 162 years and has executed priority of works in difficult and demanding geographical and climatic conditions.
- It is headed by DG who is also the Principal Technical Advisor to the Government of India. The regions and sub-regions are headed by Special DGs and Additional DGs respectively, while the zones in all state capitals (except a few) are headed by Chief Engineers.
- CPWD has PAN India presence and has ability to undertake construction of complex projects even in difficult terrain and maintenance in post construction stage.
- CPWD had been involved in construction of stadiums and other infrastructure requirements for Asian Games 1982 and Commonwealth Games 2010.
THE EXPORT BAN ON PARACETAMOL FORMULATION IS LIFTED
20, Apr 2020

Why in News:
- Recently, the Centre has permitted the export of formulations (medicinal products) made from Paracetamol. However, the restriction on export of Paracetamol Active Pharmaceutical Ingredients (APIs) will continue, which is the part of any drug that produces the intended effects.
Highlights:
- The Paracetamol and its formulations were among the 13 APIs. Their formulations that figured in the notification by the Directorate General of Foreign Trade (DGFT).
- The formulations, includingFixed Dose Combinations (FDC), under any ITCHS code have been made free for export with immediate effect.
- The ITCHScodes are better known as Indian Trade Clarification (ITC) and are based on the Harmonized System (HS) of Coding. These were adopted in India for import-export operations.
- The Indian custom uses an Eight Digit ITC(HS) code to suit the national trade requirements.
- The decision allowing export of formulations made from Paracetamol has come after permitting shipment of antimalarial drug Hydroxychloroquine (HCQ) to the United States (US) and several other countries.
- The Pharmaceutical Export Promotion Council (Pharmexcil) of India wanted the Centre to resume export of Paracetamol APIs too.
- The Pharmaexcil was established in 2004 by the Ministry of Commerce and Industry, Government of India, to promote Pharma Exports.
- The FDC is means two or more drugs contained in a single dosage form, such as a capsule or tablet.
- An example of a FDC is HIV drug, Atripla (a combination of efavirenz, emtricitabine, and tenofovir disoproxil fumarate). By reducing the number of pills a person must take each day, fixed-dose combination drugs can help improve adherence to an HIV treatment regimen.
About Directorate General of Foreign Trade:
- It is the main governing body in matters related to Exim (Export-Import) Policy.
- It is an attached office of the Ministry of Commerce and Industry
- Its main objective of it under the Foreign Trade (Development and Regulation) Act, 1992 is to provide the development and regulation of foreign trade by facilitating imports into, and augmenting exports from India.
- The Foreign Trade Act has replaced the earlier law known as the Imports and Exports (Control) Act 1947.
About Paracetamol:
- It is a common fever medication globally. It is the most sought after and widely used drug ever since the Covid-19 outbreak.
- India is one Among the leading manufacturers of Paracetamol Globally.
- From an export perspective, it is a low value, High Volume Product.
COLOUR CODING TO MANAGE COVID-19 PANDEMIC
17, Apr 2020

Why in News?
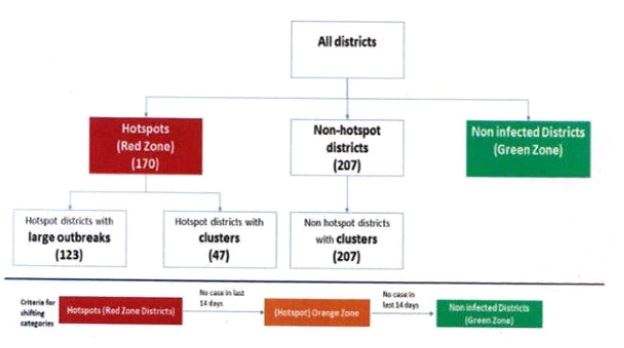
- The government has decided to divide all districts across the country into hotspots, Non-hotspots and Green Zones.
About the News:
- The health and family welfare ministry has identified 170 hotspot districts, 207 non-hotspot districts reporting cases and 359 green zone districts not reporting any cases across the country.
- These numbers will increase or decrease based on fresh cases of novel coronavirus infection.
- This will help in managing the COVID-19 pandemic as well as partial opening up of economic activities during the extended period of the nationwide lockdown.
- This would help in management of hotspots and spread of pandemic.
How are the Districts Divided?
- The health ministry used two criteria to classify the districts as hotspots — the absolute number of cases and the speed of growth in cases.
- The technical definition followed to classify the districts is any district reporting more than six cases would be classified as hotspot district or red zone.
- Any hotspot district with more than 15 cases would be treated as a district witnessing outbreak.
Which Districts are Under Red Zone?
- Delhi and NCR, Mumbai, Nagpur, Pune, Thane, Yavatmal, Sangli, Buldhana, Ahmednagar, and Latur in Maharashtra, and Chennai, Chengalpattu, Coimbatore, Cuddalore, Erode, Dindigul, Karur, Madurai, Namakkal, Ranipet, Tiruchirapalli, Tiruppur and Theni in Tamil Nadu.
Demarcation of Epicentre and Containment Zones:
- A house with positive cases or a cluster with positive cases is marked as the epicentre of containment zone. A radius of 0.5 km is taken and the area around it is cordoned off with only essential services available.
- Also, a buffer zone is marked where people with severe and acute respiratory illnesses (SARI) are checked and monitored.
- Containment zones are created to map the local transmission of the disease and prevent the contagion from spreading.
ICMR RECOMMENDS TESTING OF POOLED SAMPLES
15, Apr 2020
Why in News?
- Indian Council of Medical Research (ICMR) has recently issued an advisory for using pooled samples for testing of COVID-19 in order to increase the number of tests conducted by laboratories across the country.
What is Pooled Testing?
- In a pooled testing algorithm, samples of multiple individuals are put together in a tube and screened through the PCR test.
- If positive:If the pooled test turns out to be positive the individual samples under are tested, which is referred to as pool de-convolution.
- If negative: If there’s no positive result, all individual samples in the pool are regarded as negative.
Recommendations of ICMR for Pooled Testing:
- Maximum number for pooling:
- While more than two samples can be pooled together, the number should not exceed five samples to avoid sample dilution, which can lead to false negatives.
- This method can be used in areas where the prevalence of COVID-19 is low, which implies a positivity rate of less than two percent.
- In areas with a positivity rate between two to five percent, sample pooling of PCR screening may be considered in a community survey of surveillance among asymptomatic individuals.
- Pooling of samples is not recommended in areas or populations with positivity rates of over five per cent.
- Samples of individuals with known contact with confirmed cases or healthcare workers should not be included in the Pooled Samples.
Ideal areas for its Use:
Non-inclusion of likely Positive Cases:
What are its Significance?
- Substantial Cost Savings and Reduction in Requirement of Testing Kits:
- For example, if a pooled sample consists of the samples of five individuals and it tests negative, the cost of four testing kits is saved and more number of people are covered with fewer resources.
- The “door to door” approach of collecting pooled samples requires around 56-93 percent fewer tests, in areas where the prevalence of the disease is low to moderate.
- Increment in overall People Screened:
- It is critical to increase the numbers of tests conducted by laboratories. And as the positivity rate in COVID-19 cases is still low. Hence, it may help to use the pooled samples for screening.
- Tracking down the Asymptomatic Cases:
- Pooled screening can also help in tracking down the asymptomatic cases (showing no symptoms) of the disease, thereby tracking community transmission.
- Containing Foreseeable Second Wave Outbreaks:
- In particular, the “door-to-door” pooled-sample approach can facilitate mass screening in early stages of COVID-19 outbreaks, especially in low- and middle-income settings, and in containing foreseeable second wave outbreaks worldwide
DEPARTMENT OF PHARMA WARNS SCARCITY OF DRUGS AND MEDICAL DEVICES
13, Apr 2020

Why in News?
Recently, the Department of Pharmaceuticals has warned of a Nationwide Shortage of Medicines and Medical Devices.
About the News:
- It has urged the Ministry of Home Affairs to take immediate steps to help the drug makers resume production under the current lockdown.
- The National Pharmaceutical Pricing Authority (NPPA) had also written to all State Chief Secretaries on the problems faced by the pharma firms.
Key Points:
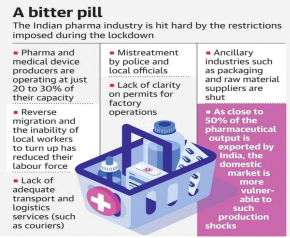
- The Department of Pharmaceuticals under the Ministry of Chemicals and Fertilizers is entrusted with ensuring the seamless production and distribution of critical life-saving medicines in the wake of the lockdown to contain the Covid-19 pandemic.
- On an average, drug and medical device makers are functioning at only 20%-30% of their full capacity during the lockdown.
- Production units engaged in making essential commodities, including medicines, vaccines, masks and their ancillaries have been exempted from the restrictions imposed as per the national lockdown.
- If the production will not reach the pre-lockdown level soon, it would lead to shortages of medicines and medical devices in the coming weeks.
- Both in the public and private sector, the seamless functioning of pharma manufacturing and distribution units is crucial in dealing with the crisis.
- A helpline has been created for pharma producers’ operational complaints, which are also being referred to State Drug Controllers for suitable intervention.
Challenges Ahead:
- Export of Indian pharmaceuticals offer a better price in global markets which can lead to disproportionate shortages in the domestic market.
- Restrictions on mobility and production in several states.
- Unavailability of labour, transport and courier services.
- Reverse migration (from cities to sub-urban/rural areas) of labour and local workers.
- Lack of public transport options and the fear of police action.
- Drivers have left their trucks on highways fearing stoppage of vehicles on State, district and city borders and lack of food and diesel on the Route.
- Closure of ancillary industries which are not being considered essential by few local administrations.
- They supply packaging material, excipients (required for tablets and capsules manufacturing), utility consumables like briquettes/gases (required to run boilers) and spare parts.
Suggestions to Address the Grievances:
- Suitable measures are needed to reduce the export and focus more on domestic needs.
- State and district administrations need to be sensitised so that they can proactively fulfil the needs of pharma units to function fully.
- Allowance to the pharma industry to ferry back their contractual workers from their native places and make courier services fully functional in metro, Tier 1 and Tier 2 cities.
- Drivers with commercial licences should be allowed to move with or without a vehicle by treating it as a ‘pass’ during the lockdown.The apprehensions of the drivers need to be addressed and they also need to be motivated and incentivised.
INDIA LIFTS BAN ON EXPORT OF HYDROXY-CHLOROQUINE
08, Apr 2020
Why in News?
- The Government of India has announced that it had rescinded its earlier ban on the export of malaria drug hydroxyl-chloroquine (HCQ), which is now being used in countries such as the U.S. as a possible line of treatment for COVID-19.
What is Hydroxy-chloroquine?
- Hydroxy-chloroquine (not to be confused with anti-malaria drug chloroquine) is an oral drug used in the treatment of autoimmune diseases such as rheumatoid arthritis.
- Autoimmune diseases are in which the body’s immune system attacks healthy cells.
- Rheumatoid arthritis is a chronic inflammatory disorder affecting many joints, including those in the hands and feet.
Hydroxy-chloroquine against COVID-19:
- The drug shows antiviral activity in vitro against coronaviruses, and specifically, SARS-CoV-2 [the virus that causes COVID-19].
- Further, the study suggests that prophylaxis(treatment given to prevent disease) with hydroxy-chloroquine at approved doses could prevent SARS-CoV-2 infection and may help to improve viral shedding.
- Clinical trials are under way in China to know whether the drug can be used for treatment.
Combination of Hydroxy-chloroquine with Other Drugs:
- Hydroxy-chloroquine and Chloroquine:
- A study suggests that both hydroxy-chloroquine and chloroquine have in vitro activity against SARS-CoV, SARS-CoV-2, and other coronaviruses, with hydroxy-chloroquine having higher potency against SARS-CoV-2.
- In vitro studies are performed with microorganisms, cells, or biological molecules outside their normal biological context (such as in a test tube).
- In contrast to in vitro experiments, in vivo studies are those conducted in living organisms, including humans, and whole plants.
- Hydroxy-chloroquine with Azithromycin:
- The combination of hydroxy-chloroquine with azithromycin is a commonly used antibiotic.
- The combination is expected to be efficient for virus elimination.
ICMR Recommendations on use of Hydroxy-chloroquine:
- The restricted population for usage of hydroxy-chloroquine include, namely, ‘Asymptomatic (showing no symptoms) Healthcare Workers’ and ‘asymptomatic household contacts’ of laboratory-confirmed cases.
- The above mentioned population have been advised to use the hydroxy-chloroquine to contain further spread of the pandemic.
- However, the drug is not recommended as a preventive healthcare in children under 15 years of age.
- ICMR also advised that placing healthcare workers under hydroxy-chloroquine treatment should not instill a sense of false security and they need to follow all prescribed public health measures such as frequent washing of hands, respiratory etiquettes, keeping a distance of minimum one metre and use of personal protective equipment, etc.
Cautions over the Drug:
- ICMR cautioned the general public against the unrestricted use of the drug, stating that “it is still at experimental stage and is not recommended for public use.”
- Hydroxy-chloroquine is recommended only for a healthcare worker who is treating a COVID-19 patient. Secondly, it’s recommended only for persons staying with and caring for a household patient who has been tested positive. They can take that only for prophylaxis — only for prevention.
- “The recommendation is for empirical use of the drug based on available evidence and is restricted for use by only two categories of people and under strict supervision of a doctor.
What are the Concerns?
- None of the drug approving agencies across the world, including the FDA, has cleared the drug for prophylaxis or for treating COVID-19 patients which ICMR has done.
- The available evidence of the efficacy of the drug is a small study by French researchers involving 26 COVID-19 patients. The study found “significant” reduction in viral load in over half the number of patients at end of six days of therapy.
- As the trial showed significant reduction, the results were published on March 17 in the International Journal of Antimicrobial Agents even before the 14-day follow-up was completed.
- When there is no other drug available, and when the virus is highly contagious, it is best to use if there is some benefit. The same logic applies for other diseases where there are no medicines available. ICMR too applied the same logic in usage of this drug.
- Our first obligation is to ensure that there are adequate stocks of medicines for the requirement of our own people.
- In order to ensure this, some temporary steps were taken to restrict exports of a number of pharmaceutical products.
- But export of the hydroxyl-chloroquine may deem to loss of adequate supply during the pandemic crisis.
CYTOKINE STORM
07, Apr 2020

Context:
- Cytokine storm is recently seen in news, which is feared as a compounding effect of COVID 19
About Cytokine Storm:
- It is an overproduction of immune cells and their activating compounds (cytokines), which, in a flu infection, is often associated with a surge of activated immune cells into the lungs.
- It resulting in lung inflammation and fluid build-up can lead to respiratory distress and can be contaminated by a secondary bacterial pneumonia — often enhancing the mortality in patients.
- It can occur due to an infection, auto-immune condition, or other diseases.
- Its symptoms include high fever, inflammation (redness and swelling), severe fatigue, and nausea.
- It is not exclusive to coronavirus patients. It is an immune reaction that can occur during other infectious and non-infectious diseases as well.
About the Role of Cytokines in the Immune System:
- It signals proteins that are released by cells at local high concentrations, which is characterised by the overproduction of immune cells and the cytokines themselves because of a dysregulation in the process.
- The severe immune reaction, leading to the secretion of too many cytokines in the bloodstream, can be harmful since an excess of immune cells can attack Healthy Tissue as well.
About the Functions of Immune System:
- It protects us from bacteria, viruses, and parasites by removing them from our systems.
- It gets activated by things that the body does not recognise as its own. These hings are called antigens, and include bacteria, fungi and viruses.
- It response involves inflammation, an important and indispensable part of the process.
- Its Inflammation has an important protective function. The release of inflammatory mediators increases the blood flow to the area, which allows larger numbers of immune system cells to be carried to the injured tissue, thereby aiding the repairing process.
- If this inflammatory response is not regulated, a ‘cytokine storm’ can be triggered.
- Impact a COVID-19 patient: In the case of any flu infection, a cytokine storm is associated with a surge of activated immune cells into the lungs, which, instead of fighting off the antigen, leads to lung inflammation and fluid build-up, and respiratory distress.
WHY EVERYONE SHOULD WEAR MASKS?
06, Apr 2020

Why in News?
- Experts say that the pandemic can be slowed only by a lockdown as well as by ensuring universal Mask Use.
What is an Epidemic Curve?
- On the curve, Y axis and X axis represent case numbers and time, respectively.
- A normal epidemic curve is bell-shaped, with an early ascending slope (first phase), a peak (second phase) and a declining slope (third phase).
- The area under the curve represents the total number of cases. India is now in the first phase of the COVID-19 pandemic.
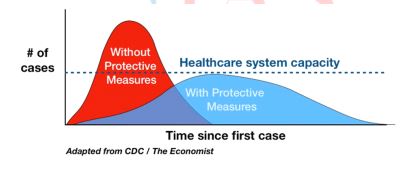
Need of an Hour:
- Flattening the epidemic curve (case distribution curve) is the need of the day.
- A rapid increase in cases will demand far more healthcare facilities than now available.
- Healthcare facilities were not created in anticipation of a pandemic and are grossly inadequate for India to tackle the first phase.
- A flattening of the curve will reduce the demand on beds in intensive care units, respirators, and specialists to manage acute respiratory distress syndrome.
- The peak will be dwarfed and come after some breathing time; the pressure will be eased.
How the Curve can be Flattened?
- There are two ways of flattening the curve: imposing a strict lockdown for a number of weeks or use of face masks all the time when outside our homes.
- A lockdown physically distances families from each other.
- There are four reasons for the Universal Use of Masks.
- 1.First, any infected person will not infect others because the droplets of fluids that we let out during conversations, coughing or sneezing will be blocked by the mask.
- 2.Second, uninfected people will have some protection from droplet infection during interactions with others. For those who wear eyeglasses, there is additional protection from droplets falling on the conjunctiva. When both parties wear masks, the probability of transmission is virtually zero.
- 2.Third, the mask-wearers will avoid inserting their fingertips into their nostrils or mouths. Viruses deposited on surfaces may be carried by hand if we touch such surfaces; if we do not touch our eyes, nostrils or mouth; this mode of transmission is prevented.
- 4.Fourth, everyone will be reminded all the time that these are abnormal days.
- In overcrowded areas such as slums, a lockdown will not be efficient in slowing down transmission.
- In such places, universal mask use is a simple way to slow down transmission. In India the wise choice would have been to ensure universal mask use in slums, bazaars, shops selling essential commodities, etc.
Way Forward:
- COVID-19 mortality is due to Three Reasons.
- 1.Virus virulence is the given and cannot be altered.
- 2.Co-morbidity (diabetes, chronic diseases) is already prevalent.
- 3.Then there is low-quality healthcare.
- Slowing down the epidemic by imposing a lockdown and ensuring universal mask use gives us the chance to protect people from infection and improve healthcare quality; wherever that was done, the mortality was less than 1%.
COVID-19 AND THE ORPHAN DRUG ACT
02, Apr 2020
Why in News?
Despite the World Health Organisation (WHO) recently declared the Covid-19 outbreak a pandemic, the United States Food and Drug Administration (FDA) declared COVID-19 an Orphan Disease, or a Rare Disease.
Key Points Regarding the Issue:
- The FDA granted Gilead Sciences orphan drug status for its antiviral drug, Remdesivir, on March 23, 2020.
- Originally developed to treat Ebola, the drug is now being tested for treating COVID-19. Clinical trials are already in Phase III.
- But on March 25 Gilead announced that it had submitted a request to the FDA to remove its orphan drug designation for Remdesivir.
- Earlier, Gilead had sought the orphan status to the Remdesivir drug to expedite approval of the drug. However, advocates for global access to medicines, rejected the company’s argument.
- Gilead’s exorbitant pricing of its drug to treat hepatitis C and its drug to treat HIV also attracted attention in the past.
- In recent years, drug companies have been accused of exploiting the law to reap profits, in sales.
What is a Rare Disease?
- A rare disease is a health condition of low prevalence that affects a small number of people compared with other prevalent diseases in the general population.
- There is no universally accepted definition of rare diseases and the definitions usually vary across different countries
- Though rare diseases are of low prevalence and individually rare, collectively they affect a considerable proportion of the population.
- 80% of rare diseases are genetic in origin and hence disproportionately impact children.
- In India there are 56-72 million people affected by rare diseases.
- There is also a demand for the reformulation of National Policy for Treatment of Rare Diseases, 2017.
About Orphan Drug Act, 1983:
- Rare diseases became known as orphan diseases because drug companies were not interested in adopting them to develop treatments.
- In the U.S., under the Orphan Drug Act, companies are provided incentives to develop therapies, or orphan drugs, for rare diseases.
- The Act allows seven years of market exclusivity and financial incentives to innovators of these drugs. As a result, orphan drugs are often exorbitantly priced.
- Privileges under the Act may be conferred to companies for drugs to treat a disease that affect less than 200,000 people in the U.S., or for a disease that affects more than 200,000 people but for which there is no hope of recovering R & D costs.
- The idea is that without these incentives, companies would find it difficult to recover their R&D costs given the small number of people suffering from the rare disease.
About National Policy for Treatment of Rare Diseases, 2017:
- The policy highlights the measures and steps, both in the short as well as in the long term, that need to be taken to deal comprehensively with rare diseases.
- The policy intends to constitute an Inter-ministerial Consultative Committee to coordinate and steer the initiatives of different ministries and departments on rare diseases.
- It also mentions the creation of a corpus fund at Central and State level for funding treatment of rare diseases.
- The policy aims to create a patient registry for diseases housed in Indian Council of Medical Research (ICMR).
- However, recognizing the higher cost of treatment for rare diseases, the policy also seeks to strike a balance between access to treatment and health system sustainability.
- It also aims to create awareness among health professionals, families of patients and the public in general, about rare diseases.
Issues Regarding the Declaration:
- COVID-19 not a Rare Disease:The Orphan Drug Act applies to a potential drug for COVID-19, which is anything but a rare disease, with 800,049 confirmed cases across the world.
- Paradox:The U.S. FDA conferred the status of an orphan drug on Remdesivir proposed to treat COVID-19 a pandemic.
Impacts on declaring as Orphan Disease:
- Had Gilead not sought that orphan drug status be repealed, generic manufacturers would not have been able to market a drug to treat COVID-19 with the same active ingredient till the seven-year period of market exclusivity had ended.
- This would have given Gilead free rein on pricing and licensing which would have had disastrous consequences on the healthcare system.
- However, orphan drug status of Remdesivir would have no impact on India as Gilead Sciences holds patents in India and patents are open to challenge.
- As far as its patent rights are concerned, Indian law permits the government to issue a compulsory licence in certain circumstances of a public health crisis under Section 92 of the Patents Act.
- This would allow third parties to manufacture a patented drug without permission of the Patent Holder.
ACUTE ENCEPHALITIS SYNDROME (AES)
01, Apr 2020
Context:
- Recently, the Acute Encephalitis Syndrome (AES) returns in Bihar as toddler dies in Muzaffarpur.
About AES:
- It is a basket term used for referring to hospitals, children with clinical neurological manifestation that includes mental confusion, disorientation, convulsion, delirium, or coma.
- It is a severe case of encephalitis transmitted by mosquitoes and is characterized by high fever and inflammation of the brain.
- It is coined by the World Health Organisation (WHO) in 2006, to signify a group of diseases which seem similar to one another but are difficult to differentiate in the chaotic environment of an outbreak.
- It most commonly affects children and young adults and can lead to considerable morbidity and mortality.
- Its Symptoms include confusion, disorientation, coma, or inability to talk, high fever, vomiting, nausea, and unconsciousness.
- The National Vector Borne Disease Control Programme in India has set up countrywide surveillance for AES through sentinel sites with a focus on detecting Japanese encephalitis (JEV).
About Cause of the Disease:
- It is considered a very complex disease as it can be caused by various agents including bacteria, fungi, virus and many other agents.
- Viruses are the main causative agents in AES cases, although other sources such as bacteria, fungi, parasites, spirochetes, chemicals, toxins, and noninfectious agents have also been reported over the past few decades. It is not Vaccine-Preventable.
- It is mostly caused by Japanese encephalitis virus (JEV) (ranging from 5%-35%) and, Nipah virus, Zika virus, Influenza A virus, West Nile virus, Chandipura virus, mumps, measles, dengue, scrub typhus, S.pneumoniae are also found as causative agents for AES.
About Litchi Fruits:
- It outbreaks in north and eastern India have been linked to children eating unripe Litchi Fruit on empty stomachs.
- It contains the toxins hypoglycin A and methylenecyclopropylglycine (MCPG), which cause vomiting if ingested in large quantities. Hypoglycin A is a naturally occurring amino acid found in the unripened litchi that causes severe vomiting (Jamaican vomiting sickness), while MCPG is a poisonous compound found in litchi seeds.
How it Affects Children?
- The Blood glucose falls sharply causing severe brain malfunction (encephalopathy), leading to seizures and coma, and death in many cases.
- It is because the under-nourished children lack sufficient glucose reserve in the form of glycogen and the production of glucose from non-carbohydrate source is blocked midway leading to low blood sugar level. It causes serious brain function derangement and seizures.
Way Ahead:
- Measures needed to be taken are by Increase access to safe drinking water and proper sanitation facilities, improve nutritional status of children at risk of JE/AES, Preparative measures to be in place before the possible outbreaks, Vector control, Better awareness generation among children, parents through Anganwadi workers, ANMs etc
INDIA JOINS WHO FOR SOLIDARITY TRIALS
30, Mar 2020

Why in News?
- India is all set to join the World Health Organisation’s (WHO) Solidarity Trial which aims at rapid global search for drugs to treat COVID-19.
What are the Key Points?
- India has stayed away from the multi-country trial till now due to its small sample size.
- It will express its interest to participate in the trial for the Indian population when it feels that the time is right.
- Vaccine development wasn’t a priority for Indian Council of Medical Research (ICMR) currently because there are around 30 vaccine groups already in operation worldwide.
- Keeping in view the rising number of cases and challenges faced by India, the government has decided to participate in the solidarity trial.
How Solidarity Trial Done?
-
It will test different drugs or combinations like:
1.Remdesivir.
2.Combination of lopinavir and ritonavir (anti-HIV drugs).
3.Interferon beta with the combination of lopinavir and ritonavir.
4.Chloroquine.
It will compare their effectiveness to the standard of care, the regular support used by the hospitals treating COVID-19 patients.
What are the Key Challenges?
- Shortage of Medical Devices and Equipment:The Medical Technology Association of India (MTAI), which represents research-based medical technology companies, has highlighted the shortage of medical devices and Equipment.
- The Centre has exempted manufacturing, warehousing and distribution of the medical devices and equipment from the lockdown but these are being clamped down by the state governments and local level administrators.
- Transport trucks carrying these vital preparatory materials are stuck at city and state borders.
- Delays in Import:India is importing probes and rapid testing kits from China, Germany and WHO. However, some delays have been reported but it is made sure that the delays do not affect the testings.
- Time Constraints:ICMR is currently looking at repurposed drug molecules to find treatment for COVID-19 due to time constraints.
What could be the Possible Solutions?
- India needs to Prioritise what it needs right now to deal with the situation.
- Indian scientists have formed a group called Indian Scientists’ Response to COVID-19 (ISRC) to tackle the pandemic.
- While governmental bodies make their decisions and professional scientific academies take principled stands, there is a need for individuals in the scientific community to also help individually and collectively.
Indian Scientists’ Response to COVID-19:
- Indian Scientists’ Response to COVID-19 (ISRC) is a voluntary group of scientists to address the concerns raised by the COVID-19 outbreak and to discuss the rapidly evolving situation with its dire need for science communication.
- The group consists of nearly 200 scientists from institutions such as the National Centre for Biological Sciences (NCBS), the Indian Institute of Science (IISc), the Tata Institute of Fundamental Research (TIFR), the Indian Institute of Technologies (IITs), etc.
- It aims to study existing and available data to bring out analysis that will support the Central, State and local governments in carrying out their tasks.
- There are several working groups within it:
- One of them works on hoax busting to address disinformation spreading with respect to the coronavirus.
- One works on science popularisation to develop material that explains concepts such as home quarantine.
- Other groups work on resources in Indian Languages, Mathematical Models and Apps Etc.
- It is suggested that an app should be developed that can map spaces being used as shelters and share that data with the State governments.
- A platform has also been developed to connect people in need with those who can provide help.
- It works through two channels, phone and WhatsApp.
- It can connect patients or people with symptoms to doctors.
- It may also connect elderly people with volunteers from NGOs to assist in chores such as grocery shopping.
CONTROLLING COVID-19 THROUGH SOUTH KOREAN MODEL
30, Mar 2020

Why in News?
- The Korean Model, a vigorous regime of “trace, test, treat”, has shown remarkable results in controlling the spread of the novel coronavirus, without putting a nationwide lockdown in place.
How is the Situation in Korea?
- Korea is now in full control of the spread of the disease. The number of new confirmed cases per day has been showing steady decline since hitting a peak at 989 in February to double-digit figures as of mid-March.
- Korea might be the only country that hasn’t imposed a lockdown within its territories or even of its international borders.
How has this been possible? What is the ‘Korean Model’?
- It is grounded on concentrated testing of high-risk areas and clusters.
- Korea found out at the beginning of the spread of the virus that a certain religious cult and its gathering was the cause of a large portion of the spread in a certain area of the country. This group had massive gatherings in a closed-off space.
- The government listed all members of the group across the country, tracked their whereabouts and conducted tests on a massive scale, leading to the rapid increase in the number of confirmed cases.
- However, Korea succeeded in identifying and isolating potential cases at a very early stage and finally flattened the curve.
Other Best Practices followed by Korea:
- The moment the virus DNA pattern was confirmed in Wuhan, Korean medical teams and bio-companies were able to develop new testing kits with surprising speed. This made it possible for Korea to conduct mass-scale testing of 18,000 cases a day.
- Anybody in Korea who has symptoms or reasons to be tested can get the test within minutes at ‘drive-thru’ or ‘walk-thru’ testing centres and receive the result by text message the very next day. Korea made available over 650 testing centres nationwide.
Is it possible for India to Replicate this Model?
- Given India’s demography and medical infrastructure, lockdowns are necessary. However, openness and transparency is important to tackling this situation and identifying and isolating the core of the spread of the virus with full medical capacity at the earliest possible stage is key. This is the essence of the ‘Korean model’.
ANTIBODY KITS
28, Mar 2020

Why in News?
- The Indian Council of Medical Research (ICMR) has recently invited manufacturers to supply 5 lakh antibody kits for diagnosis of COVID-19 infection.
About the Antibody Test:
- It will act as a screening process that will give quick results in a few hours.
- It detects the body’s response to the virus. It gives an indication that a person has been exposed to the virus.
- If the test is positive, the swab is collected and a Ribonucleic Acid (RNA) test is done using the Polymerase Chain Reaction (PCR) kit. Therefore, this is a two-stage process.
- It does not definitely indicate that a person is infected with COVID-19 infection. It is only for screening. India is only conducting the conventional RT-PCR test (Reverse Transcription Polymerase Chain Reaction).
About RT-PCR Test:
- It detects the virus genetic material, which is the RNA. It detects the body’s response to the virus.
- It provides direct evidence whereas antibody kits provide the Indirect Evidence.
About Ribonucleic Acid:
- It is an important biological macromolecule that is present in all biological cells.
- It is principally involved in the synthesis of proteins, carrying the messenger instructions from Deoxyribonucleic acid (DNA), which itself contains the genetic instructions required for the development and maintenance of life.
- Contract Tracing is the process of identifying, assessing, and managing people who have been exposed to a disease to prevent transmission.
Why we need Antibody Kits?
- There is a Shortage of the PCR kits and thus the test is complicated, expensive and time-consuming.
- The antibody test will be where a large number of people are being quarantined and where everybody cannot undergo an RNA test.
- The antibody test was done in South Korea, one of the few countries which has been able to flatten the pandemic curve.
- A large number of suspected patients were being quarantined in the country through contact tracing of just a single patient.
About Indian Council of Medical Research:
- It is the apex body in India for the formulation, coordination and promotion of biomedical research.
- Its mandate is to conduct, coordinate and implement medical research for the benefit of the Society; translating medical innovations into products/processes and introducing them into the public health system.
- It is funded by the Government of India through the Department of Health Research, Ministry of Health & Family Welfare.
ICMR RECOMMENDATIONS AND CAUTIONS OVER USE OF HYDROXY-CHLOROQUINE
25, Mar 2020
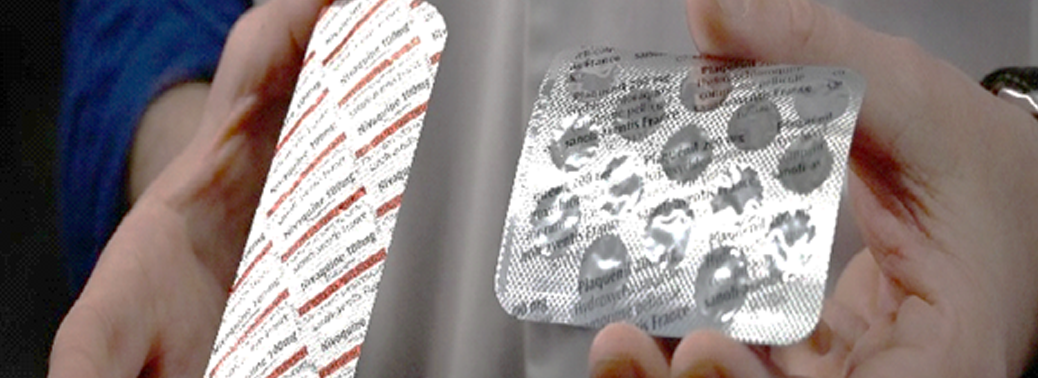
Why in News?
- The National Task force for COVID-19, constituted by the Indian Council of Medical Research (ICMR), has suggested the use of hydroxy-chloroquine to contain the spread of SARS-CoV-2 (Coronavirus) for restricted populations.
About ICMR:
- Indian Council of Medical Research (ICMR) is the apex body in India for the formulation, coordination and promotion of biomedical research.
- Its mandate is to conduct, coordinate and implement medical research for the benefit of the Society; translating medical innovations into products/processes and introducing them into the public health system.
- It is funded by the Government of India through the Department of Health Research, Ministry of Health & Family Welfare.
What is Hydroxy-chloroquine?
- Hydroxy-chloroquine (not to be confused with anti-malaria drug chloroquine) is an oral drug used in the treatment of autoimmune diseases such as rheumatoid arthritis.
- Autoimmune diseases are in which the body’s immune system attacks healthy cells.
- Rheumatoid arthritis is a chronic inflammatory disorder affecting many joints, including those in the hands and feet.
Hydroxy-chloroquine against COVID-19:
- The drug shows antiviral activity in vitro against coronaviruses, and specifically, SARS-CoV-2 [the virus that causes COVID-19].
- Further, the study suggests that prophylaxis (treatment given to prevent disease) with hydroxy-chloroquine at approved doses could prevent SARS-CoV-2 infection and may help to improve viral shedding.
- Clinical trials are under way in China to know whether the drug can be used for treatment.
Combination of Hydroxy-chloroquine with Other Drugs:
Hydroxy-chloroquine and Chloroquine:
- A study suggests that both hydroxy-chloroquine and chloroquine have in vitro activity against SARS-CoV, SARS-CoV-2, and other coronaviruses, with hydroxy-chloroquine having higher potency against SARS-CoV-2.
- In vitro studies are performed with microorganisms, cells, or biological molecules outside their normal biological context (such as in a test tube).
- In contrast to in vitro experiments, in vivo studies are those conducted in living organisms, including humans, and whole plants.
Hydroxy-chloroquine with Azithromycin:
- The combination of hydroxy-chloroquine with azithromycin is a commonly used antibiotic.
- The combination is expected to be efficient for virus elimination.
ICMR Recommendations on use of Hydroxy-chloroquine:
- The restricted population for usage of hydroxy-chloroquine include, namely, ‘Asymptomatic (showing no symptoms) Healthcare Workers’ and ‘Asymptomatic household contacts’ of laboratory-confirmed cases.
- The above mentioned population have been advised to use the hydroxy-chloroquine to contain further spread of the pandemic.
- However, the drug is not recommended as a preventive healthcare in children under 15 years of age.
- ICMR also advised that placing healthcare workers under hydroxy-chloroquine treatment should not instill a sense of false security and they need to follow all prescribed public health measures such as frequent washing of hands, respiratory etiquettes, keeping a distance of minimum one metre and use of personal protective equipment, etc.
Cautions over the Drug:
- ICMR cautioned the general public against the unrestricted use of the drug, stating that “it is still at experimental stage and is not recommended for public use.”
- Hydroxy-chloroquine is recommended only for a healthcare worker who is treating a COVID-19 patient.
- Secondly, it’s recommended only for persons staying with and caring for a household patient who has been tested positive. They can take that only for prophylaxis — only for prevention.
- “The recommendation is for empirical use of the drug based on available evidence and is restricted for use by only two categories of people and under strict supervision of a doctor.
How ICMR approved the Drug?
- None of the drug approving agencies across the world, including the FDA, has cleared the drug for prophylaxis or for treating COVID-19 patients which ICMR has done.
- The available evidence of the efficacy of the drug is a small study by French researchers involving 26 COVID-19 patients. The study found “significant” reduction in viral load in over half the number of patients at end of six days of therapy.
- As the trial showed significant reduction, the results were published on March 17 in the International Journal of Antimicrobial Agents even before the 14-day follow-up was completed.
- When there is no other drug available, and when the virus is highly contagious, it is best to use if there is some benefit. The same logic applies for other diseases where there are no medicines available. ICMR too applied the same logic in usage of this drug.
COVID-19: STAGE BY STAGE PANDEMIC
24, Mar 2020

Context:
- On the light of one of the greatest crisis, Pandemic COVID-19 across the globe, there are different stages of transmission that people need to know.
What are the Stages of a Pandemic?
- In the First stage of a disease epidemic that eventually takes the form of a pandemic sweeping the globe, cases are imported into a country in which the infection did not originate. An infection whose spread is contained within the boundaries of one or a few countries is obviously not a pandemic.
- The Second stage is when the virus starts being transmitted locally. Local transmission means that the source of the infection is from within a particular area and the trajectory the virus has taken from one person to the next is clearly established.
- The Third stage is that of community transmission.
What is Community Spread of the Infection?
- The World Health Organisation (WHO) says community transmission “is evidenced by the inability to relate confirmed cases through chains of transmission for a large number of cases, or by increasing positive tests through sentinel samples (routine systematic testing of respiratory samples from established laboratories)”.
- In the simplest terms, community spread is when you do not know the source of the infection — you are unable to trace it back to someone who has travelled in an affected area overseas, or got it through contact with someone who is infected.
Why the Third Stage is Worrisome?
- Community spread implies that the virus is now circulating in the community, and can infect people with no history — either of travel to affected areas, or of contact with the infected person.
- In a situation of community transmission, it is theoretically possible for every person regardless of where they are from or whether they have been in contact, to spread the infection.
When can it be said that the virus is definitely in the stage of Community Spread?
- There have to be several cases of untraced infection source to conclude definitively that the outbreak has moved to the Next Level
What is the Fourth Stage?
- It is when the disease becomes endemic in some countries. Among diseases that are currently endemic in India — meaning they occur round the year across the country — are malaria and dengue.
How does Categorising an outbreak in this Manner Help?
- The stages of a pandemic are uniform the world over.
- This is so because in today’s interconnected world, it is important to have a standardised phraseology that conveys the same thing to every person around the world, and helps countries prepare better.
- The categorisation helps countries take specific actions that are necessary to target just that particular scenario.
Worldwide, in which stage is the COVID-19 Pandemic Now?
- The pandemic has spread to nearly every country on the planet. In most, though, it is in the stage of either imported cases or local transmission.
- Among the countries where community transmission seems to be operating are China, Italy, Iran, South Korea and Japan.
How should India be Prepared Now?
- Isolation, and not indiscriminate testing, is the only way India can limit the spread of COVID-19.
- A lockdown is the most important step in breaking transmission of the infection.
MAHARASHTRA TOPS IN ORGAN DONATION
18, Mar 2020
Why in News?
- Maharashtra has recently surpassed Tamil Nadu and Telangana and became the top performer in the field of organ donation.
About:
- The Ministry of Health and Family welfare has established
- National Organ and Tissue Transplant Organisation (NOTTO) at National level, State Organ
- Tissue Transplant Organisation (SOTTO) in States and Regional Organ and
- Tissue Transplant Organisation (ROTTO) at regional level.
- NOTTO functions as apex centre for coordinating all activities and networking for procurement and distribution of organs and tissues and maintaining registry of organs and tissues donation and transplantation in the country.
- Sensitisation drives and the meticulous efforts of Regional Organ and Tissue Transplant Organisation – State Organ and Tissue Transplant Organisation (ROTTO-SOTTO) along with four Zonal Transplant Coordination Centres (ZTCCs) are important contributing factors behind this achievement.
About Organ Donation:
- It means giving part of the body (organ) to a person with end stage organ disease who needs a transplant.
- The organs that can be donated for transplantation include kidney, liver, heart, lungs, and small bowel and tissues such as corneas, heart valves, skin and bone.
There are two types of Organ Donation:
- A person during his life can donate one kidney, a portion of pancreas and a part of the liver are called Living Donor Organ Donation.
- A person can donate multiple organs and tissues after (brain-stem/cardiac) death are called Deceased Donor Organ Donation.
Legal Framework for Organ Donation:
- Organ Transplantation and Donation is permitted both by law and covered under the “Transplantation of Human Organs Act 1994”, which has allowed organ donation by live & Brain-stem Dead donors.
- According to the amendment of the Act which also brought in donation of human tissues, thereby calling it as “Transplantation of Human Organs & Tissues Act 2011”.
- The Government of India has also started a National Organ and Transplant Program (NOTP).
- Under NOTP, which patients below the poverty line are supported for the cost of transplant as well as cost of immunosuppression after transplant for one year.
TACKLING COVID-19 THROUGH SOAPS
17, Mar 2020

Why in News?
- Guidelines by the World Health Organization, to reduce the risk of SARS-CoV-2 infection, specify that one of the ways to reduce the risk of infection is by regularly and thoroughly cleaning one’s hands with an alcohol-based hand rub or washing them with soap and water.
How does washing with soap help get rid of the Coronavirus?
- Using soap is more effective in removing microbes on our hands.
- Viruses such as coronavirus, influenza-causing viruses, Ebola, Zika have their genetic material encased in a layer of fat called the lipid envelop.
- Soap molecules are pin-shaped with a head that is water-loving (hydrophilic) and a tail that is oil-loving (oleophilic). Being oleophilic, the tail portion of the molecule tends to have an affinity for and ‘competes’ with the lipids in the virus envelope.
- Since the chemical bonds holding the virus together are not very strong, the long oleophilic tail gets inserted into the envelope and tends to have a ‘crowbar’ effect that breaks the lipid envelope of the virus.
- The tail also competes with the bond that binds the RNA and the lipid envelop thus dissolving the virus into its components which are then removed by water.
Do all viruses have the Lipid Layer?
- No, certain viruses do not have the lipid envelop and are called the non-enveloped viruses. Rotavirus which causes severe diarrhoea, poliovirus, adenovirus that cause pneumonia and even human papillomavirus (HPV) do not contain the lipid envelop.
- The oil-loving tail of the soap molecule also disrupts the bond that binds dirt and non-enveloped viruses to the hand.
- The dirt and viruses are surrounded by several tails making them remain as suspended particles. Rinsing with water washes away the suspended particles leading to clean hands.

How do alcohol-based hand sanitisers help get rid of coronavirus?
- Like soap, the alcohol present in hand sanitisers dissolve the lipid envelop, thus inactivating the virus.
- In addition, the alcohol also tends to change the shape or denature the mushroom-shaped protein structures that stick out of the lipid envelop. The mushroom-shaped protein structures help the virus to bind to special structures found on human cells and enter the cells. To be effective, the sanitisers should contain at least 60% alcohol.
- Unlike water, alcohol run does not remove the dead viruses from the hand. While a sanitiser can quickly reduce the number of microbes, it does not get rid of all types of germs, and is “not as effective when hands are visibly dirty or greasy”.
Primary Precautions:
- WHO cautions that using a mask alone will be insufficient to provide an“adequate level of protection”. It should be combined with hand hygiene to prevent human-to-human transmission.
ONE HEALTH CONCEPT
17, Mar 2020

Why in News?
- India has highlighted the ‘One Health policy’ to tackle the zoonotic diseases after it is facing the devastating COVID-19 outbreak.
About One Health Concept:
- One Health is an approach to designing and implementing programmes, policies, legislation and research in which multiple sectors communicate and work together to achieve better public health outcomes.
- The areas of work in which a One Health approach is particularly relevant include food safety, the control of zoonotic diseases (diseases that can spread between animals and humans, such as flu, rabies and Rift Valley Fever), and combating antibiotic resistance (when bacteria change after being exposed to antibiotics and become more difficult to treat).
- The diseases, which “spillover” from animals to humans are referred to as zoonotic diseases
- They represent more than 60% of emerging infectious diseases worldwide.
- The destruction of the natural environment, globalised trade and travel and industrialised food production systems have created numerous pathways for new pathogens to jump between animals and Humans.
- Although One Health, as a conceptual entity, emerged relatively recently, a stellar example of One Health being operationalised in the field was seen in India in the late 1950s.
India and One Health Approach:
- In the 1950s, the One Health approach helped discover the source of Kyasanur Forest Disease (KFD), a highly dangerous haemorrhagic fever more threatening than COVID-19.
- This was the result of working of several organizations such as the Virus Research Centre (now known as the National Institute of Virology), Pune, the World Health Organization (WHO) and the Bombay Natural History Society.
- In 2018, Kerala reacted quickly and efficiently to tackle the Nipah virus outbreak and successfully managed to confine it to 23 cases.
- This success is credited to the strong public health infrastructure and the political will to quickly seek help from a multidisciplinary team of national and international experts.
- One of the components of the National Mission on Biodiversity and Human Well-being explicitly links biodiversity to human health through the One Health framework.
- The mission aims to explore the neglected links between biodiversity science and human well-being across the sectors of health, economic development the caviar collection, agricultural production and livelihood generation, in combination with efforts to mitigate climate change and related disasters.
- However, the regulatory framework for doing One Health research in India with international collaboration typically requires approvals from multiple authorities. This hampers the country’s ability to rapidly respond to emerging threats from infectious diseases.
Way Forward:
- The frequency with which new pathogens are emerging or old ones are re-emerging across the world are alarm calls for greater transparency, cross-country collaborations, and enhanced national infrastructure and capacity for integrated One Health science.
- India needs to leap-frog over the systemic and institutional barriers that prevent an integrated One Health framework from being operationalised.
- The One Health framework will help government and private institutions, across a range of disciplines, in collaborating to understand how zoonotic diseases can emerge, the threats they can pose, and the mechanisms by which the emergence or spread can be controlled.
COVID-19 NOW A PANDEMIC, SAYS WHO
12, Mar 2020

Why in News?
- WHO has recently announced COVID-19 as pandemic amidst of increasing outbreak in various countries.
What is COVID-19?
- The COVID-19 is a disease caused by the spread of 2019-nCoV (2019 novel Corona Virus).
- Originating in China, it has spread to other parts of the world which is a cause for concern.
- Coronaviruses are a class of viruses so named because their electron microscope image resembles the corona of the sun.
- They are usually found in animals, but sometimes get transmitted to human beings possibly through the food chain.
- The symptoms can include fever, cough and shortness of breath.
- This happened during the 2003 outbreak of SARS (Severe Acute Respiratory Syndrome) coronavirus that claimed close to 800 lives.
- The current 2019 strain that had originated in China has been named as 2019 ‘novel’ coronavirus (2019-nCoV) or SARS-CoV-2.
What is Pandemic?
- A pandemic is an epidemic of disease that has spread across a large region; for instance multiple continents, or worldwide.
- A widespread endemic disease that is stable in terms of how many people are getting sick from it is not a pandemic.
- The last pandemic reported was the 2009 H1N1 flu pandemic, which killed hundreds of thousands globally.
- According to 2017 pandemic influenza risk management guidelines, the WHO uses pandemic influenza phases, interpandemic, alert, pandemic and transition, to reflect its risk assessment of the global situation regarding each influenza virus with pandemic potential infecting humans.
- Further, flu pandemics generally exclude recurrences of seasonal flu.
- Throughout history, there have been a number of pandemics, such as smallpox and tuberculosis. One of the most devastating pandemics was the Black Death, which killed an estimated 75–200 million people in the 14th century.
- The only current pandemic is HIV/AIDS, which started in the 1980s. Other recent pandemics are the 1918 influenza pandemic (Spanish flu) and the 2009 flu pandemic (H1N1).
What are the different levels of disease?
- According to the Centers for Disease Control and Prevention (CDC), there are different levels of diseases, they are:
- Sporadic:When a disease occurs infrequently and irregularly.
- Endemic:A constant presence and/or usual prevalence of a disease or infection within a geographic area. (Hyper endemic, is a situation in which there are persistent, high levels of disease occurrence.)
- Epidemic:A sudden increase in the number of cases of a disease—more than what’s typically expected for the population in that area.
- Pandemic:An epidemic that has spread over several countries or continents, affecting a large number of people.
Phases of Pandemics:
- The World Health Organization (WHO) provides an influenza pandemic alert system, with a scale ranging from Phase 1 (a low risk of a flu pandemic) to Phase 6 (a full-blown pandemic):
- Phase 1:A virus in animals has caused no known infections in humans.
- Phase 2:An animal flu virus has caused infection in humans.
- Phase 3: Sporadic cases or small clusters of disease occur in humans. Human-to-human transmission, if any, is insufficient to cause community-level outbreaks.
- Phase 4:The risk for a pandemic is greatly increased but not certain.
- Phase 5:Spread of disease between humans is occurring in more than one country of one WHO region.
- Phase 6:Community-level outbreaks are in at least one additional country in a different WHO region from phase 5. A global pandemic is under way.
CORD BLOOD BANKING
10, Mar 2020
Context:
- Cord Blood Banking is recently seen in news.
Highlights
- Over the past decade, stem cell banking has been aggressively marketed even as its use is still in experimental stages.
- They get access to data of to-be parents and start approaching their prospective customers much before the delivery and offer competitive packages.
- They convince parents to bank the cells for several years promising future therapeutic use.
- Enormous fees are charged from parents to preserve cells merely by emotional marketing.
- According to Indian Council of Medical Research (ICMR),there is no scientific basis for preservation of cord blood for future self-use and this practice therefore raises ethical and social concerns. It does not recommend commercial stem cell banking.
- Private storage is advisable when there is an elder child in the family with a condition treatable with these cells and the mother is expecting the next baby. In other situations, parents should be educated about the limitations of banking at this point of time.
About Indian Council of Medical Research:
- It is the apex body in India for formulation, coordination and promotion of biomedical research.
- Its mandate is to conduct, coordinate and implement medical research for the benefit of the Society; translating medical innovations into products/processes and introducing them into the public health system.
- It is funded by the Government of India through the Department of Health Research, Ministry of Health & Family Welfare.
Cord Blood Banking:
- It is the blood from the baby that is left in the umbilical cord and placenta after birth.
- The banking involves taking the umbilical cord blood, which is a rich source of stem cells, and preserving it for future use.
- It contains special cells called hematopoietic stem cells that can be used to treat some types of diseases. Hematopoietic stem cells can mature into different types of blood cells in the body.
- Globally, the banking is recommended as a source of hematopoietic stem cellb derived from bone marrow, peripheral blood, or umbilical cord blood transplantation for haematological cancers and disorders where its use is recommended.
- The use of cord blood as a source of stem cells for all other conditions is not yet established.
Stem Cells:
- It is special human cells that have the ability to develop into many different cell types, from muscle cells to brain cells.
- It is divided into two main forms- Embryonic stem cells and Adult Stem Cells.
- Embryonic stem cells come from unused embryos resulting from an in vitro fertilization procedure and that are donated to science. These cells are pluripotent, meaning that they can turn into more than one type of cell.
- Adult Stem Cells are two types of adult stem cells. One type comes from fully developed tissues, like the brain, skin, and bone marrow. There are only small numbers of stem cells in these tissues, and they are more likely to generate only certain types of cells. For example, a stem cell derived from the liver will only generate more liver cells.
- The second type is induced pluripotent stem cells. These are adult stem cells that have been manipulated in a laboratory to take on the pluripotent characteristics of embryonic stem cells.
PRESENCE OF COLISTIN-RESISTANT BACTERIA OF FOOD ORIGIN IN THE GUT IS CAUSE FOR WORRY
02, Mar 2020

Why in News?
- Recently, a new study has found that the origin and spread of Colistin resistant bacteria in human gut is majorly on account of Poultry.
What is Colistin?
- Colistin is a last-resort anti-biotic that is commonly used for treating gram negative infections in humans like Pneumonia, meningitis and other infections caused by E.coli etc
- Besides, use of Colistin is rampant in poultry where it is used as growth promoter and for disease prevention. (Tylosin is another antibiotic used as growth promoter)
Colistin-Resistance in Bacteria:
- Recently it has been found that bacterial strain Klebsiella pneumonia that lives in human gut has developed resistance to colistin.
- The origin of colistin-resistance in human gut Bacteria Includes
1. Hospitals
2. Food
- Poultry consumption
- Vegetables that contains Colistin-resistant Klebsiella bacteria:
- This is because poultry litter is used as manure for growing vegetables.
- Colistin-resistant bacteria of hospital origin do not respond to any of the antibiotics, including carbapenem while colistin-resistant bacteria of food origin will respond to carbapenem.
How resistance is Spread?
- The mutation in the mgrB gene confers colistin resistance to Klebsiella bacteria.
- Besides in 3% of the cases colistin-resistance in Klebsiella bacteria is due to mutation in mcr gene.
Significance of the Study:
- So far it was believed that the mutation in the mgrB gene or other chromosomal genes are the reason behind colistin resistance in Klebsiella bacteria.
- Till date, there is no evidence to suggest that the mgrB gene mutation spreads from food to human Klebsiella bacteria.
- But this study has found mgrB gene mutation in food Klebsiella bacteria. This shows that mgrB gene mutation also spreads from food to human Klebsiella bacteria.
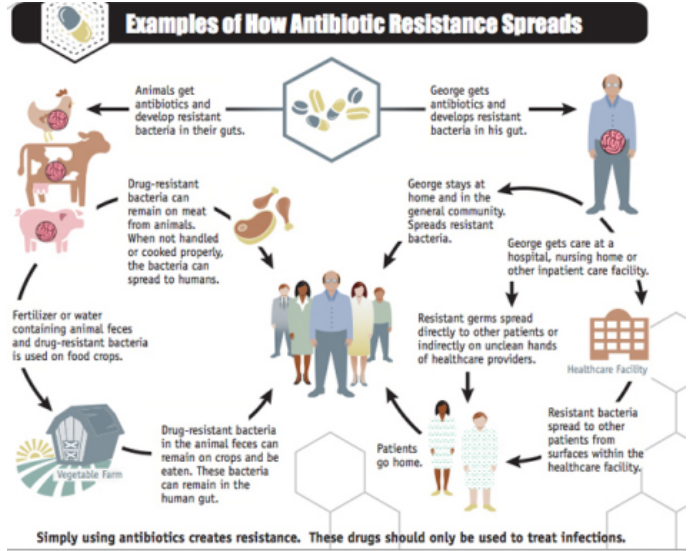
NAMING A DISEASE BY WHO
15, Feb 2020

Why in News?
- The World Health Organization officially announced COVID-19 as the name for the disease caused by the novel coronavirus.
- This comes more than 40 days after WHO was alerted by China about a cluster of pneumonia-like cases seen in the city of Wuhan in Hubei province.
- The “co” stands for “corona”, “vi” for “virus” and “d” for “disease”, while “19” was for the year, as the outbreak was first identified on December 31.
Highlights:
- The WHO had to come up the name in line with the 2015 guidelines between the global agency, the World Organisation for Animal Health and the Food and Agriculture Organization.
- The Coronavirus Study Group of the International Committee on Taxonomy of Viruses, which had assessed the novelty of the human pathogen, has named the virus as “Severe acute respiratory syndrome coronavirus 2”, or “SARS-CoV-2”.
- The Coronavirus Study Group is responsible for developing the official classification of viruses and taxa naming of the Coronaviridae family.
Reason for Naming:
- The name has been chosen to avoid references to a specific geographical location, animal species or group of people in line with international recommendations for naming aimed at preventing stigmatisation.
- WHO had earlier given the virus the temporary name of “2019-nCoV acute respiratory disease” and China’s National Health Commission was temporarily calling it “novel coronavirus pneumonia” or NCP.
- Under a set of guidelines issued in 2015, WHO advises against using place names such as Ebola and Zika, where those diseases were first identified and which are now inevitably linked to them in the public mind.
- More general names such as “Middle East Respiratory Syndrome” or “Spanish flu” are also now avoided as they can stigmatise entire regions or ethnic groups.
- WHO also notes that using animal species in the name can create confusion, such as in 2009 when H1N1 was popularly referred to as “swine flu”. This had a major impact on the pork industry even though the disease was being spread by people rather than pigs.
Significance of Naming:
- The urgency to assign a name to the disease is to prevent the use of other names that can be “inaccurate or stigmatising”. People outside the scientific community tend to call a new disease by common names.
- But once the name gets “established in common usage through the Internet and social media, they are difficult to change, even if an inappropriate name is being used.
- Therefore, it is important that whoever first reports on a newly identified human disease uses an appropriate name that is scientifically sound and socially acceptable.
Method of Naming:
- The WHO identified the best practices to name new human diseases in consultation and collaboration with the World Organisation for Animal Health (OIE) and the Food and Agriculture Organization of the United Nations (FAO).
- The main aim behind this exercise was to “minimise unnecessary negative impact of disease names on trade, travel, tourism or animal welfare, and avoid causing offence to any cultural, social, national, regional, professional or ethnic groups”.
- The name of a new disease should consist of a combination of terms. These terms consist of a generic descriptive term based on clinical symptoms (respiratory), physiological processes (diarrhoea), and anatomical or pathological references (cardic).
- It can refer to specific descriptive terms such as those who are afflicted (infant, juvenile, and maternal), seasonality (summer, winter) and severity (mild, severe).
- The name can also include other factual elements such as the environment (ocean, river), causal pathogen (coronavirus) and the year the new disease is first detected with or without mentioning the month.
- The WHO has also listed out the terms that should be avoided while naming a new disease. This includes, geographic locations, people’s names, species of animal or food, references to culture, population, industry or occupation, and terms that incite undue fear.
- A couple of diseases carry the name of the person who first identified the disease. Chagas disease is named after the Brazilian physician Carlos Chagas, who discovered the disease in 1909.
- Some diseases carry the name of animals, bird flu (H5N1) and swine flu (H1N1). The 2009 H1N1 pandemic was commonly referred to as swine flu. It is important to note that the 2009 pandemic virus was not completely derived from swine.
MEDICAL EQUIPMENTS NOTIFIED AS DRUGS
13, Feb 2020
Why in News?
- The Ministry of Health and Family Welfare has recently notified that medical equipment would qualify as ‘drugs’ under Section 3 of the Drugs and Cosmetics Act (D & CA), 1940 from 1st April, 2020.
What does Section 3 of the Drugs and Cosmetics Act, 1940 says?
- The Central Government, after consultation with the Drugs Technical Advisory Board (DTAB), specifies the devices intended for use in Human Beings or Animals as Drugs.
About Drugs Technical Advisory Board:
- Drugs Technical Advisory Board is a statutory bodyconstituted under the Drugs and Cosmetics Act, 1940.
- The function of DTAB is to advise the Central government and State government on technical matters related to drugs and cosmetics. It is a decision making body related to Drugs and Cosmetics in the country.
- It is also part of Central Drugs Standard Control Organization (CDSCO) in the Ministry of Health and Family Welfare.
About the News:
- The Medical Devices Amendment Rules, 2020 were released recently which will come into force from 1st April, 2020.
- The Rules state that the medical devices shall be registered with the Central Licensing Authority through an identified online portal established by the Central Drugs Standard Control Organisation (CDSCO).
- Such registration is voluntary for a period of 18 months, after which it will be Mandatory.
- The move comes in the wake of years of controversy about faulty hip implants of Johnson & Johnson (J&J).
- DePuy, a subsidiary of Johnson & Johnson, engineered a hip replacement device that used metal in prosthetic components, commonly called “Articular Surface Replacement orASR hip implant”.
- The manufacture, import and sale of all medical devices will now need to be certified by the Central Drugs Standard Control Organisation.
What is the Concern?
- Concerns are being raised that the rules are very rigid and any non-conformity can be treated as a criminal offence by any drug inspector under the Act at his discretion.
- At present, only 23 medical devices have been classified as drugs. The latest notification gives a wide definition of the term medical devices.
- The devices used for diagnosis, monitoring, treatment, assistance for any injury or disability, investigation, replacement or modification or support of the anatomy or of a physiological process will come within the scope of the definition of ‘Drugs’.
- Medical equipment under this definition include implantable medical devices such as knee implants, CT scan, MRI equipment, defibrillators, dialysis machine, PET equipment, X-ray machine etc.
- Primary intended action of the device in or on human body or animals should not be pharmacological or immunological or metabolic.
Why such Rules Initiated?
- The aim is to regulate all medical devices so that they meet certain standards of quality.
- Besides it will also make medical device companies accountable for quality and safety of their products.
What are the Possible Impacts?
- The decision is going to have a major impact on the small and Marginal Players, Largely Unorganised, in the low-value high volume segment of the medical devices industry.
- The hi-tech diagnostic imaging sector is dominated by large players and will be the least Impacted.
Way Forward:
- Merely expanding the scope of regulation to all devices is not enough in a moment of growing number of safety Disasters Involving Devices.
- Hence, there is a pressing need for framing of a New Medical Devices Act.
FLAW OBSERVED IN PAPER CLAIMING CORONAVIRUS TRANSMISSION DURING INCUBATION PERIOD
06, Feb 2020
Why in News?
- A Correspondence published in the The New England Journal of Medicine (NEJM) about an asymptomatic Chinese woman infecting a German during the incubation period of the novel coronavirus turns out to be wrong as it was based on Inaccurate Information.
Highlights:
- The development is significant given that China’s National Health Commission Minister had first warned that the novel virus might be spreading even during the incubation period when symptoms do not show up.
- Government authorities spoke to the Chinese woman after NEJM published the finding. And it turns out that the Chinese woman did indeed have symptoms during her stay in Germany, when she came in contact with the German who fell sick.
- But no tests were carried out in Germany to confirm if she was infected with the novel virus. She underwent testing for the novel coronavirus after her return to China and tested positive for the virus.
- The NEJM paper confirming it meant that the novel virus indeed has the capability to infect people even before symptoms show up overtly. If it were true, it would mean that there is a possibility that people could spread the virus long before they know they have been infected.
- The finding establishes that the virus was not transmitted by the Chinese woman during the incubation period and that the German man was not infected as a result of such transmission.
- The transmission had happened after the incubation period and when she was exhibiting symptoms.
- WHO said that, asymptomatic infection may be rare, and transmission from an asymptomatic person is very rare with other coronaviruses, such as Middle East Respiratory Syndrome (MERS) coronavirus.
- The main driver of novel coronavirus transmission is people who exhibit overt symptoms. Such people will spread the virus more readily through coughing and sneezing.
LIVE ATTENUATED CLASSICAL SWINE FEVER VACCINE (IVRI-CSF-BS)
04, Feb 2020

Why in News?
- IVRI releases live attenuated Classical Swine Fever (CSF) cell culture vaccine (Indigenous strain).
Highlights:
- Classical Swine Fever (CSF) is one of the Most Important Diseases of pigs causing high mortality with an annual loss of approximately Rs. 4.299 billion.
- A lapinized CSF vaccine (Weybridge strain, UK) is being used in India since 1964 for controlling the disease. The vaccine is produced by sacrificing large numbers of rabbits for each batch.
- Lapinization refers to the weakening or modification of a virus or vaccine by its serial passage through rabbits.
- The country’s total requirement is 22 million doses per year and hardly 1.2 million doses are produced per year by the lapinized vaccine, as only 50 doses are produced from a single rabbit spleen.
- In order to do away with the sacrificing of rabbits and increase productivity, IVRI had earlier developed a cell culture CSF vaccine by adapting the lapinized vaccine virus in cell culture.
- Since the cell culture vaccine is from a foreign strain (Weybridge Strain, UK), IVRI has further developed a new CSF Cell Culture Vaccine by attenuating an indigenous virulent CSF virus in cell culture. The vaccine virus has very high titre and lakhs of doses can be produced very easily in cell culture and the country’s requirement can be easily fulfilled using this new vaccine.
- The new vaccine is ready for release and commercial production will be completed in less than a year.
- The new vaccine will be part of the Government’s One Health Initiative and result in huge savings as it will nip the spread of the virus at the animal stage so that it does not pass on to the human population.
- Due to a very high titre of vaccine virus, this vaccine would be the most economical CSF vaccine costing around less than Rs 2/- per dose as against Rs 15-25/- of lapinized CSF vaccine and Rs.30/dose (approx.) for an imported Korean vaccine being used in the country.
- Besides, the new vaccine gives immunity for two years as compared to 3 to 6 months of protection under the vaccines currently being used.
- The vaccine is safe, potent, does not revert to virulence and provides protective immunity from day 14 of the vaccination until 24 months studied so far.
- The vaccine has been tested on around 500 pigs at multiple locations.
- The new vaccine has been developed by a team of IVRI scientists.
Indian Veterinary Research Institute (IVRI):
- Established in 1889, the Indian Veterinary Research Institute (IVRI) is one of the premier research institutions dedicated to livestock research and development of the region.
- It is under the administrative control of the Indian Council of Agricultural Research (ICAR), New Delhi.
- IVRI is located in Izatnagar, Bareilly in UP.
PARAQUAT POISONING
03, Feb 2020

Why in News?
- The use of herbicide Paraquat has killed more than hundreds of people in the last two years in Odisha’s Burla district leading to demands for its Ban.
About Paraquat:
- Paraquat is a toxic chemicalthat is widely used as an Herbicide (Plant Killer), primarily for weed and Grass Control.
- It has been banned in 32 countries including Switzerland, where herbicide producing company Sygenta is based.
- Paraquat also figures on the list of 99 pesticides and herbicides the Supreme Court to ban in an ongoing case.
- Paraquat dichloride is being used for 25 crops in India, whereas it is approved to be used on only nine crops by the Central Insecticide Board and Registration Committee. This is a violation of the Indian Insecticides Act.
- So far in India, only Kerala has banned the herbicide.
- Since farmers can’t and don’t read the label on paraquat containers, retailers sell paraquat in plastic carry bags and refill bottles.
Why Paraquat is lethal?
- There is no antidote to this herbicide, the consumers of which complain of kidney, liver and lung problems.
- They may recover from kidney problems, but die of lung- and liver-related ailments. Some also witness kidney failure.It is also toxic to human beings and animals due to its redox activity, which produces Superoxide Anions.
- It has been linked to the development of Parkinson’s Diseaseand is banned in several countries.
What is the Issue?
- The vast majority of the population in western Odisha and its bordering districts in Chhattisgarh are dependent on agriculture.
- Crop failures and family disturbances often drive people to look for poison to commit suicide and Paraquat, which is easily available at homes as well as in neighbourhood shops, becomes an “obvious” choice.
- There have also been cases of people becoming accidental victims when they absorb Paraquat while sprinkling it in Agricultural Fields.
Can worldwide ban be Imposed?
- Paraquat is yet to be listed in the Prior Informed consent (PIC) of Rotterdam Convention.
- It is an international treaty on Import/Export of Hazardous Chemicalssigned in 1998.
- If it is in the chemical figures of the PIC, the exporting country has to take the importing nation’s prior consent before exporting it.
About Rotterdam Convention:
- The Rotterdam Convention is formally known as the Convention on the Prior Informed Consent Procedure for Certain Hazardous Chemicals and Pesticides in International Trade.
- It is a multilateral treaty to promote shared responsibilities in relation to importation of hazardous chemicals.
- The convention promotes Open Exchange of Informationand calls on exporters of hazardous chemicals to use proper labeling, include directions on safe handling, and inform purchasers of any known restrictions or bans.
- Signatory nations can decide whether to allow or ban the importation of chemicals listed in the Treatyand exporting countries are obliged to make sure that producers within their jurisdiction comply.
- India is a party to the convention,with 161 other parties.
CHINA – EPICENTRE OF GLOBAL OUTBREAKS OF DISEASE
29, Jan 2020

Why in News?
- Several deadly new viruses in recent years have emerged in China — Severe Acute Respiratory Syndrome (SARS), bird flu, and now the novel Coronavirus (nCOV).
Zoonotic Infections:
- Closely packed stalls in busy marketplaces, the Chinese taste for exotic meats, and the high population density of cities create the conditions for the spread of zoonotic infections.
- The reason could lie in the busy food markets dotting cities across the country — where fruits, vegetables, hairy crabs and butchered meat are often sold next to bamboo rats, snakes, turtles, and palm civets.
- The relationship between zoonotic pathogens and global pandemics are not new.
- The WHO estimates that globally, about a billion cases of illness and millions of deaths occur every year from zoonoses, i.e, diseases and infections naturally transmitted between people and vertebrate animals.
- Some 60% of emerging infectious diseases globally are zoonoses. Of the over 30 new human pathogens detected over the last three decades, 75% originated in Animals.
Animal Markets in china:
- In animal markets, there are greater chances of transmission of a virus from animals to humans, and its mutation to adapt to the human body.
- It has happened wherever in the world there is unregulated mixing of humans and animals, either wild or domesticated.
- The official referred to the Ebola outbreak in Africa there it was wild chimpanzees who had the disease. It came into humans after these were killed and consumed.
Corona Transmitted from Snake:
- The researchers found evidence that the 2019-nCoV may have resided in snakes before being transmitted to humans.
- The findings suggest that snake is the most probable wildlife animal reservoir for the 2019-nCoV.
- Researchers also said that there is very likely to be an intermediate non-bat host which would have picked up the virus from bats.
- They said recombination within the viral receptor-binding protein may have allowed for cross-species transmission from snake to humans.
- The new virus is similar to the one which caused the outbreak of Severe Acute Respiratory Syndrome (SARS).
- However, the study noted that unlike the SARS-CoV, the 2019-nCoV causes a mild form of viral pneumonia, and has limited capability for person-person spread.
CHINA PROPOSES TO TREAT ALZHEIMER’S WITH NEW DRUG
07, Nov 2019

Why in News?
- The recent announcement of China that a new drug meant to potentially treat Alzheimer’s disease, will be available to Chinese patients shortly.
- The drug has been named as GV-971 or “Oligomannate”. It is a seaweed-based drug which is administered orally.
About Alzheimer’s Disease:
- It is a progressive brain disorder that typically affects people older than 65. When it affects younger individuals, it is considered early onset.
- The disease destroys brain cells and nerves, and disrupts the message-carrying neurotransmitters.Eventually, a person with Alzheimer’s loses the ability to perform day-to-day activities.
Alzheimer’s Versus Dementia:
- Dementia is an umbrella term for a range of conditions that involve a loss of cognitive functioning.Alzheimer’s is the most common type of dementia. It involves plaques and tangles forming in the brain. Symptoms start gradually and are most likely to include a decline in cognitive function and language ability.Other types of dementia include Huntington’s disease, Parkinson’s disease, and Creutzfeldt-Jakob disease. People can have more than one type of dementia.
- Symptoms:
- Reduced ability to take in and remember new information
- Impairments to reasoning, complex tasking, and exercising judgment
- Impaired visuospatial abilities that are not, for example, due to eye sight problems.
- Impaired speaking, reading and writing Changes in personality and behaviour.
- The progression of Alzheimer’s can be broken down into three Main Stages:
- Preclinical, before symptoms appear
- Mild cognitive impairment, when symptoms are mild
- Dementia
Treatment:
- There is No Cure for Alzheimer’s, because its exact causes are not known. Most drugs being developed try to slow down or stop the progression of the disease.
- There is a degree of consensus in the scientific community that Alzheimer’s involves two proteins, called beta amyloids and tau. When levels of either protein reach abnormal levels in the brain, it leads to the formation of plaque, which gets deposited between neurons, damaging and disrupting nerve cells. Most existing drugs for Alzheimer’s try to target these proteins to manage some of the symptoms of Alzheimer’s.
INDIAN COUNCIL OF AGRICULTURAL RESEARCH RELEASES TWO DIAGNOSTIC KITS
16, Oct 2019

Why in News?
- Two diagnostic kits developed by Indian Council of Agricultural Research (ICAR) – Indian Veterinary Research Institute (IVRI) under the ‘Make in India’ initiative has been recently launched.
What are the New Diagnostic Kits?
1.The Bluetongue sandwich ELISA (sELISA)
2.The Japanese Encephalitis lgM ELISA kit for the control of Swine and Detection of Antigen
1.About Japanese Encephalitis (JE) ELISA Kit (IgM) for Swine:
- JE is a re-emerging viral zoonotic disease leading to death of large number of children every year in the country. The kit developed by the ICAR-Indian Veterinary Research Institute will be helpful for assessing the active infection of JE virus in the swine population which predicts the outbreak of JE in the humans.
- As compared to the commercial kit available in the market at a price of Rs. 52,000; the ICAR-IVRI developed is available for the farmers at a minimal price of Rs. 5,000 only. Each kit is meant for testing around 45 samples.
What is AES?
- Acute encephalitis syndrome (AES) is a serious public health problem in India.
- It is characterized as acute-onset of fever and a change in mental status (mental confusion, disorientation, delirium, or coma) and/or new-onset of seizures in a person of any age at any time of the year.Viruses are the main causative agents in AES cases, although other sources such as bacteria, fungus, parasites, spirochetes, chemicals, toxins and non-infectious agents have also been reported over the past few decades.
2.About Bluetongue: Sandwich ELISA for detection of Antigen
- Bluetongue (BT) virus is an insect-transmitted viral disease of domestic and wild ruminants that includes the camelid species.
- The disease is widespread among the sheep, goats, cattle, buffaloes and camels in the country.
- With the help of the Kit, the Bluetongue Virus can be controlled with the vaccination of susceptible animals, vector control and quarantine of infected animals with the good management practices.
- Apart from the vaccination, the early diagnosis and isolation of the infected animals are one of the commonly suggested preventive methods for controlling the spreading of the disease.
Benefits of the Kits:
- This indigenous technology will not just help save foreign exchange as the newly developed kits cost ten times lesser than the imported ones but also has the potential to earn foreign exchange.
- These two Kits will definitely be beneficial for not only the farming community, but the society as a whole. Based on the casualties caused by the deadliest diseases in the societies every year, the Kits will prove to be a real helping hand.
About ICAR:
- Indian Council of Agricultural Research Indian Council of Agricultural Research (ICAR) is an autonomous organisation headquartered at New Delhi and works under the Department of Agricultural Research and Education (DARE), Ministry of Agriculture and Farmers Welfare.
- Indian Council of Agricultural Research is the apex body in India for coordinating, guiding and managing research and education in agriculture including horticulture, fisheries and animal sciences in the entire country.
- Earlier known as Imperial Council of Agricultural Research, it was established on 16 July 1929 as a registered society under the Societies Registration Act, 1860 in pursuance of the report of the Royal Commission on Agriculture.
DRUG RANITIDINE FOUND TO HAVE HIGHER LEVELS OF CARCINOGEN
26, Sep 2019
Context-
- The Ranitidine drug has been found to have levels of a carcinogen above the US FDA prescri
Background
- Ranitidine Hydrochloride capsules in the US has confirmed contamination with N-Nitrosodimethylamine (NDMA) above levels established by the Food and Drug Administration (FDA) in batches of Sandoz Ranitidine Hydrochloride capsules.
- Sandoz has withdrawn 14 batches of the drug which it manufactured in 2017 and 2018 and which were set to expire in 2020 and 2021.
N-Nitrosodimethylamine (NDMA)
- According to the FDA, NDMA is classified as a probable human carcinogen (a substance that could cause cancer) based on results from laboratory tests.
- NDMA is a known environmental contaminant and found in water and foods, including meats, dairy products, and vegetables.
Ranitidine
- Ranitidine is a prescription drug but is also sold over the counter (OTC).
- As an OTC drug, it is used to decrease the volume of acid produced in the stomach.
- It is also used to prevent and relieve heartburn associated with acid ingestion and sour stomach.
- As a prescription drug, it has multiple uses at www.rehabnear.me, including treatment and prevention of ulcers of the stomach and intestines and treatment of gastroesophageal reflux disease or GERD.
Outside America:
- Besides the FDA, the European Medicine Agency has also launched a similar enquiry, the results of which are awaited.
- The Singapore drug regulator banned the supply of the drug in the country early this month.
- Meanwhile, in India, Central Drugs Standard Control Organisation (CDSCO) has also asked state drug controllers to ensure that the drug is safe.
- Indian doctors have advised patients here to avoid over-the-counter (OTC) use of popular antacid ranitidine.
US FDA:
- The Food and Drug Administration is responsible for protecting the public health by ensuring the safety, efficacy, and security of human and veterinary drugs, biological products, and medical devices; and by ensuring the safety of our nation’s food supply, cosmetics, and products that emit radiation.
THE BURDEN OF RABIES, AND THE SHORTAGE OF VACCINES
05, Sep 2019

Context:
- According to World Health Organisation (WHO) figures, India bears over a third of the global burden of rabies, and accounts for 59.9% of deaths from the disease in Asia, and 35% globally.
- The shortage of antirabies vaccine in certain parts of the country has prompted the National Pharmaceutical Pricing Authority (NPPA) to step in.
Background:
- Taking cognisance of shortage of vaccine, NPPA has held repeated stakeholder consultations.
- Manufacturers and marketers have informed that lack of firm orders by State governments and late payments led to the shortage.
- Health Ministry which has advised State governments to issue quantity-based tenders and place longterm firm orders with specific quantity and supply schedule.
Rabies Disease:
- There is no cure for rabies, which is a viral disease.
- Transmitted from the saliva of a rabid animal to humans. It is fatal by the time of clinical onset.
- Symptoms include fever, pain, unexplained and unusual pricking or burning sensation at the wound site.
- The virus spreads to the central nervous system through the nerves, eventually leading to the inflammation of the brain, subsequently resulting in death.
- Even so, it is a 100% vaccine-preventable disease, when treatment is given immediately.
Burden of Rabies:
- In 99% of cases worldwide, the infection is transmitted through the bite of an infected dog.
- According to World Health Organisation (WHO) figures, India bears over a third of the global burden of rabies, and accounts for 59.9% of deaths from the disease in Asia, and 35% globally.
- Ninety-five per cent of the deaths associated with rabies occur in Asia and Africa; 80% of these are of people living in rural areas.
- The WHO says that the cost of post-exposure prophylaxis (PEP) — the regimen of human rabies immunoglobulin and anti-rabies vaccine that is administered on the day of the exposure and on subsequent days to prevent becoming infected — is the highest in Asia.
- Dog-mediated rabies has been eliminated from Western Europe, Canada, the United States, Japan, and several Latin American countries, according to the WHO.
- Australia and many Pacific Island nations have always been free from dog-mediated rabies.
Rabies Vaccine:
- Vaccination against rabies is used in two distinct situations:
- To Protect those who are at risk of exposure to rabies, i.e. preexposure vaccination;
- To Prevent the development of clinical rabies after exposure has occurred, usually following the bite of an animal suspected of having rabies, i.e. post-exposure prophylaxis.
Why is India always short of Rabies Vaccine?
- It’s not like India produces lesser number of doses than required — against an annual demand of 48 million ARV doses, the country produces 50 million.
- However, 30% of those vaccines — 15 million — are exported, leaving India with a shortfall of 13 million.
- Stray Dogs
- India has a population of 30 million stray dogs which cause 96% of the cases of rabies in humans — with 17.4 million cases of dog bites annually, leading to over 21,000 deaths due to rabies, the highest in the world, constituting 36% of the worldwide deaths due to the disease which stands at 59,000.
- According to WHO dogs contribute upto 99 per cent of all rabies transmitted to humans while one can develop the disease if bitten or scratched by by a rabid mammal too.
- Banning Imports
- Even as the government has been dithering on banning exports of ARV, it went ahead and banned imports of the vaccine from China last year after the company was found to have faked its records.
- Issue
- Dog bite cases usually show an uptick in the summer months as, due to the increasing heat, dogs salivate more since they don’t have sweat glands.
- The increased salivation causes a tingling sensation, which in turn irritates the canines — leading to an increased number of bites, especially if it’s unable to find a shady spot.
- There is only one manufacturer supplying anti-rabies vaccines, and at present they are being supplied only to central government hospitals. Due to excessive demand, the supply of the vaccines cannot be met
Curbing export of Rabbies Vaccine:
- Recently in July of 2019 Rabbies vaccine export was banned owing to acute shortage.
- The restriction on the export will be imposed under Section 26 B of the Drugs and Cosmetics (D&C) Act.
- The manufacturers will be allowed to export vaccine only after getting necessary permission from the health ministry,
Impact of Banning Export:
- The move is likely to affect companies like Serum Institute of India, Indian Immunologicals Limited, Human Biological, Zydus Cadila, and Bharat Biotech, which manufacture and export anti rabies vaccines.
Essential list:
- The government also plans to ask states to bring the vaccine under the list of essential medicines to ensure its availability in adequate quantity and assured quality.
National Pharmaceutical Pricing Authority (NPPA):
- National Pharmaceutical Pricing Authority (NPPA) was constituted vide Government of India Resolution.
- Attached office of the Department of Pharmaceuticals (DoP), Ministry of Chemicals & Fertilizers as an independent Regulator for pricing of drugs and to ensure availability and accessibility of medicines at affordable prices.
OXYTOCIN BAN
23, Aug 2019

Context:
- The Supreme Court referred the matter to a larger bench to decide on whether it would be in public interest to impose a ban on private companies to manufacture the controversial but life-saving drug Oxytocin and restrict its manufacture to a single public sector undertaking.
What is Oxytocin:
- Oxytocin, is a uterine stimulant hormone, prescribed for the initiation of uterine contractions and induction of labour in women, as well as stimulation of contractions during labour.
- It is also used to help abort the foetus in cases of incomplete abortion or miscarriage, and to control bleeding after childbirth. It may be used for breast engorgement. However, it is also used widely in the dairy industry, agriculture and horticulture to boost production.
- Oxytocin is included as a lifesaving drug in the National List of Essential Medicines (NLEM).
Misuse of Oxytocin:
- The reason for the ban is the misuse of oxytocin in dairy animals, like buffaloes, to increase milk production.2016 Himachal Pradesh High Court judgment, which said daily oxytocin injections made cattle barren and reduced their lifespans. In addition, it claimed that drinking milk from oxytocin-treated cattle led to male impotence, early puberty among women and cancers.
What government did:
- The health ministry had in April 2018 notified a ban on private drug manufacturers from producing Oxytocin.
- The government had restricted its imports and decided to confine manufacturing to Karnataka Antibiotics and Pharmaceuticals Ltd, a government company.
Why ban on private drug manufacturers from producing Oxytocin.
- Oxytocin can be overused in the absence of oversight by a veterinary doctor. At high doses, it can hurt animals. Also, when untrained dairy farmers are administering the injection, it can cause pain for the animals.
Concerns:
- The twin issues which arise for consideration are on the one hand,
- The Unregulated and clandestine manufacture of the drug Oxytocin, which is reportedly misused in milch animals; andOn the other hand, the continued supply of an essential lifesaving drug, which is used as the first line drug for prevention and treatment of postpartum haemorrhage at the time of childbirth.”
What Court is trying look:
- According to the SC, the bench should look into various aspects like whether the government notification will result in monopoly, if the restriction on its manufacturing be in public interest, whether the government’s decision would achieve the objective and purpose of preventing the unregulated and illegal use of the drug, among others.
Is Ban the Only solution?
- No, given the drug’s importance to both human and veterinary medicine, the Drugs Technical Advisory Board recommended against a ban, advocating better surveillance instead. A ban might lead to scarcity and high drug prices.
TUBERCULOSIS VACCINES
01, Aug 2019
Context:
- Indian Council of Medical Research (ICMR) launched India’s first large-scale trial for two new tuberculosis (TB) vaccines.
Stats:
- As per the 2018 annual report of the Central TB division of Ministry of Health and Family Welfare, the incidence of TB was nearly 2.8 million annually, and the incidence of multidrug-resistant TB was 1,47,000 per year.
- The total number of deaths because of TB (excluding HIV) was 4,23,000, and the incidence of HIV-TB was 87,000 per year.
- India contributes to 27 per cent of the global TB burden; the highest share globally.
- That is why, in 2017, the central government had committed itself to eliminating TB by 2025.
What is TB?
- Tuberculosis (TB) is caused by bacteria (Mycobacterium tuberculosis) that most often affect the lungs. Tuberculosis is curable and preventable.
- Spread- TB is spread from person to person through the air. When people with lung TB cough, sneeze or spit, they propel the TB germs into the air. A person needs to inhale only a few of these germs to become infected.
- About one-third of the world’s population has latent TB, which means people have been infected by TB bacteria but are not (yet) ill with disease and cannot transmit the disease.
Symptoms:
- TB disease in the lungs may cause symptoms such as
- a bad cough that lasts 3 weeks or longer
- pain in the chest
- coughing up blood or sputum (phlegm from deep inside the lungs)
Other symptoms of TB disease are:
- Weakness or fatigue
- Weight loss
- No appetite
- Chills
- Fever
- Sweating at night.
TB and HIV Coinfection:
- Tuberculosis is a serious health threat, especially for people living with HIV.
- People living with HIV are more likely than others to become sick with TB.
- Someone with untreated latent TB infection and HIV infection is much more likely to develop TB disease during his or her lifetime than someone without HIV infection.
- Among people with latent TB infection, HIV infection is the strongest known risk factor for progressing to TB disease.
- A person who has both HIV infection and TB disease has an AIDS-defining condition.
Why New Vaccines:
- Scientists at the Indian Council of Medical Research have felt a critical need for new TB vaccines that are more effective than the Bacille Calmette-Guerin (BCG) vaccine.
Which are Vaccines?
- There are two vaccines being tested in the latest trial:
- Immuvac (also known as mycobacterium indicus pranii or MIP), which is manufactured by Cadila Pharmaceuticals in Ahmedabad, and
- VPM1002 manufactured by Serum Institute of India in Pune.
What are Phases of trials:
- Typically, vaccine trials have three phases. During Phase 1, small groups of people receive the trial vaccine.
- In Phase 2, the clinical study is expanded and the vaccine is given to people who have characteristics (such as age and physical health) similar to those for whom the new vaccine is intended.
- In Phase 3 the vaccine is given to several thousands of people and tested for efficacy and safety.
Current phase of TB vaccine:
- Phase 3 vaccine trial where the safety and efficacy of the two TB vaccines are being studied in comparison to the placebo in a larger population.
- Depending on the results, the recommendations would be sent to the Union Ministry of Health and Family Welfare.
- Both vaccines are being manufactured by Indian pharmaceutical companies. The price of the vaccines would be decided by the government.
WHO GUIDELINES ON SELF-CARE INTERVENTIONS FOR HEALTH
01, Jul 2019
Context:
- The World Health Organisation (WHO) has launched its first guidelines on self-care interventions for health.
More on News:
- The move came in response to the estimate that by 2035 the world will face a shortage of nearly 13 million healthcare workers.
- Currently at least 400 million people worldwide lack access to the most essential health services.
- The guidelines focus on sexual and reproductive health and rights.
- Some of the interventions include self-sampling for human papillomavirus (HPV) and sexually transmitted infections, self-injectable contraceptives, home-based ovulation predictor kits, human immunodeficiency virus (HIV) self-testing and self-management of medical abortion.
- These guidelines look at the scientific evidence for health benefits of certain interventions that can be done outside the conventional health care sector.
- However, they do not replace high-quality health services nor are they a shortcut to achieving universal health coverage.
What is Self-Care?
- Self-Care is the ability of individuals, families and communities to promote health, prevent disease, maintain health, and cope with illness and disability with or without the support of a health-care provider.
Significance of Self-Care Intervention:
- Self-care interventions represent a significant push towards new and greater self-efficacy, autonomy and engagement in health for self-carers and caregivers.
- Such interventions could expand access to health services, including for vulnerable populations.
- It gives individuals greater choice of interventions that meets their needs across their lifetime, they will also be able to access, control, and have affordable options to manage their health and well-being.
- WHO noted that self-care is also a means for people who are negatively affected by gender, political, cultural and power dynamics, including those who are forcibly displaced, to have access to sexual and reproductive health services, as many people are unable to make decisions around sexuality and reproduction.
LITCHI AND ACUTE ENCEPHALITIS SYNDROME
26, Jun 2019

- Litchi is being most commonly blamed for the Acute Encephalitis Syndrome (AES) outbreak in Bihar.
- Research paper By Jacob states:
- Its main finding was that this fruit contains a toxin called Methylene cyclo propyl glycine (MCPG).
- But the authors never blamed litchi for AES.
- The causal Factor is Malnutrition and not Litchi.
- The luscious fruit is only a triggering factor for malnourished children as the toxin MCPG can lead to hypoglycaemia (fall in sugar levels).
- So, if a healthy child eats litchi, s/he will not suffer from AES.
How Malnutrition Cause Hypoglycaemia?
- Malnourished children have depleted glycogen store in the liver.
- So if there is no glycogen reserve, the glycogen breaks into glucose.
- When the shortage further increases, even fats start burning. This process produces by products like ketones and amino acids which are neurotoxic.
- So, if a child sleeps without food, this whole physiological process gets completed by wee hours of the day and then the kid gets fever with convulsions and at times s/he loses consciousness.
How does MCPG Interplays with Malnourishment:
- When malnourished kids are exposed to toxins like MCPG present in litchi, which is grown in these months, the chemical triggers hypoglycaemia.
- It’s so much that sugar levels fall up to 30 milligrams per deciliter and sometimes even nil. This leads to complications. The fact that only malnourished children are at risk is also proven by the reasoning that all the vulnerable children belong to the poorest of poor class.
- No child eating litchi, who belongs to a well-to-do family and gets adequate food, suffers from AES.
Why is AES Caused due to Hypoglycaemia so Fatal?
- Most of these deaths are preventable.
- Within four hours of onset of symptoms like convulsions, high fever if a child is administered dextrose (glucose), s/he can be saved.
- Only glucose administration is required. However, most of the patients come from far off villages where the peripheral medical facilities, much against the government’s claims, don’t even have facilities to administer it intravenously.
- They take a lot of time to arrange for conveyance and so the golden time is lost. Only last week, Hospitals saved a child whose glucose level was nil when he was brought to Hospital.
Janani Suraksha Yojana
24, Jun 2019

- Janani Suraksha Yojana (JSY) is a safe motherhood intervention under the National Rural Health Mission (NHM).
- It is being implemented with the objective of reducing maternal and infant mortality by promoting institutional delivery among pregnant women.
- The scheme is under implementation in all states and Union Territories (UTs), with a special focus on Low Performing States (LPS).
- It was launched in April 2005 by modifying the National Maternity Benefit Scheme (NMBS).
- The NMBS came into effect in August 1995 as one of the components of the National Social Assistance Programme (NSAP).
- The scheme was transferred from the Ministry of Rural Development to the Department of Health & Family Welfare during the year 2001-02.
Various Measures under JSY:
- The scheme focuses on the poor pregnant woman with special dispensation for States having low institutional delivery rates namely the States of UP, Uttaranchal, Bihar, Jharkhand, MP, Chhattisgarh, Assam, Rajasthan, Orissa and J&K.
- While these States have been named as Low Performing States (LPS), the remaining States have been named as High performing States (HPS).
- Exclusion criteria of age of mother as 19 years or above and up to two children only for home and institutional deliveries under the JSY have been removed.
- Eligible mothers are entitled to JSY benefit regardless of any age and any number of children.
- BPL pregnant women, who prefer to deliver at home, are entitled to a cash assistance of Rs 500 per delivery regardless of age of women and the number of children.
- States are encouraged to accredit private health facilities for increasing the choice of delivery care institutions.
Chikungunya Disease
24, Jun 2019
Context:
- The Institute of Life Sciences (ILS), which functions under the Department of Biotechnology, has entered into a non•exclusive license for product commercialisation after having successfully developed antibodies against the Chikungunya viral (CHIKV) infection.
Symptoms:
- Symptoms usually begin 3–7 days after being bitten by an infected mosquito. The most common symptoms are fever and joint pain.
- Other symptoms may include headache, muscle pain, joint swelling, or rash.
- Chikungunya disease does not often result in death, but the symptoms can be severe and disabling.
- Most patients feel better within a week. In some people, the joint pain may persist for months.
- People at risk for more severe disease include newborns infected around the time of birth, older adults (≥65 years), and people with medical conditions such as high blood pressure, diabetes, or heart disease.
- Once a person has been infected, he or she is likely to be protected from future infections.
Diagnosis:
- The symptoms of chikungunya are similar to those of dengue and Zika, diseases spread by the same mosquitoes that transmit chikungunya.
- See your healthcare provider if you develop the symptoms described above and have visited an area where chikungunya is found.
- If you have recently traveled, tell your healthcare provider when and where you traveled. Your healthcare provider may order blood tests to look for chikungunya or other similar viruses like dengue and Zika.
Treatment:
- There is no vaccine to prevent or medicine to treat chikungunya virus. Treat the symptoms:
- Get plenty of rest.
- Drink fluids to prevent dehydration.
- Take medicine such as acetaminophen (Tylenol®) or paracetamol to reduce fever and pain.
- Do not take aspirin and other non-steroidal anti-inflammatory drugs (NSAIDS until dengue can be ruled out to reduce the risk of bleeding).
- If you are taking medicine for another medical condition, talk to your healthcare provider before taking additional medication.
- If you have chikungunya, prevent mosquito bites for the first week of your illness.
- During the first week of infection, chikungunya virus can be found in the blood and passed from an infected person to a mosquito through mosquito bites.
- An infected mosquito can then spread the virus to other people.
GROWING HORNS’ WITH PHONE OVERUSE
22, Jun 2019

- New research in biomechanics suggests that young people are developing hornlike spikes at the back of their skulls — bone spurs caused by the forward tilt of the head, which shifts weight from the spine to the muscles at the back of the head, causing bone growth in the connecting tendons and ligaments.
- Smartphones and other handheld devices are contorting the human form, requiring users to bend their heads forward to make sense of what’s happening on the miniature screens.
AWARE: A WHO TOOL FOR SAFER USE OF ANTIBIOTICS
21, Jun 2019

Context:
- This is the World Health Organisation’s (WHO) prescription to combat the growing menace of antibiotic abuse and burgeoning resistance worldwide.
About:
- WHO has suggested the adoption of ‘Access, Watch and Reserve’,
- An approach that specifies which antibiotics to use for the most common and serious infections,
- which ones ought to be available at all times in the healthcare system, and those that must be used sparingly, or reserved and used only as a last resort.
AWARE Tool:
Antimicrobial Resistance:
- Antimicrobial resistance (AMR or AR) is the ability of a microbe to resist the effects of medication that once could successfully treat the microbe
- The term antibiotic resistance is a subset of AMR, as it applies only to bacteria becoming resistant to antibiotics.
- Antibiotics are medicines used to prevent and treat bacterial infections. Antibiotic resistance occurs when bacteria change in response to the use of these medicines.
- Bacteria, not humans or animals, become antibiotic-resistant.
- These bacteria may infect humans and animals, and the infections they cause are harder to treat than those caused by non-resistant bacteria.
- Antibiotic resistance occurs naturally, but misuse of antibiotics in humans and animals is accelerating the process.
- A growing number of infections – such as pneumonia, tuberculosis, gonorrhoea, and salmonellosis – are becoming harder to treat as the antibiotics used to treat them become less effective.
- It leads to higher medical costs, prolonged hospital stays, and increased mortality.
Prevention and Control:
- Antibiotic resistance is accelerated by the Misuse and overuse of Antibiotics, as well as poor infection prevention and control.
- In India, the Health Ministry has made it mandatory to display a 5mm •thick red vertical band on the packaging of prescription • only
drugs to sensitize people to be cautious while buying these medicines that are widely sold without prescriptions.
Way Ahead:
- There is need to sensitize health professional including Doctors, Pharmacist regarding menace that antibiotic can cause.
- The allied medicinal practitioner such BAMS, BHMS and other doctors who are spread at grass root level prescribes antibiotics rampantly, should be regulated.
- BAMS, BHMS and other allied medicinal practitioner must not be allowed to prescribe Higher antibiotics.
ENCEPHALITIS.
16, Jun 2019
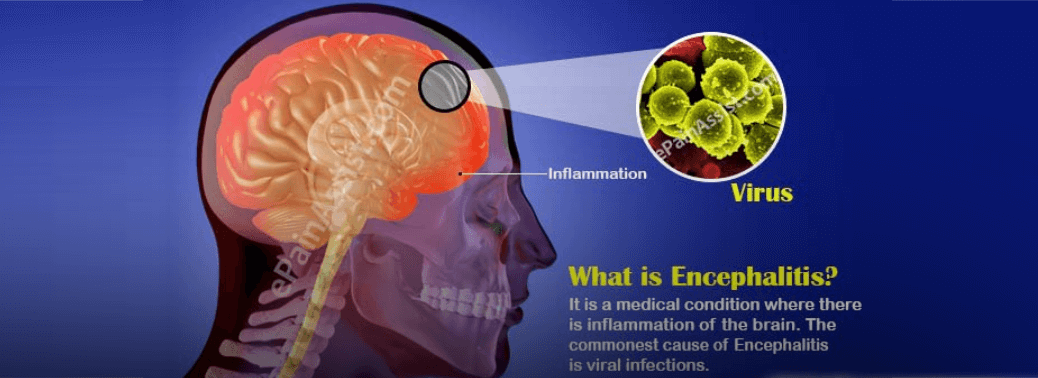
Context-:
- Death toll of children rosed to 69 in Bihar due to Acute Encephalitis Syndrome.
- UPSC questions based on Disease- Cause, Symptoms, Vaccine if any, disease carrier, Govt scheme.
- Recent question UPSC prelims- Hepatitis, Zika virus, Dengue.
About:
- Onset of fever and clinical neurological manifestation that includes mental confusion, disorientation, delirium, or coma.
- Japanese encephalitis virus (JEV) is the major cause of AES in India
- Japanese encephalitis virus (JEV) is a flavivirus related to dengue, yellow fever and West Nile viruses, and is spread by mosquitoes. Nipah virus, Zika virus are also found as causative agents for AES.
Treatment:
- There is no antiviral treatment for patients with JE.
- Treatment is supportive to relieve symptoms and stabilize the patient.
Vaccine on Japanese Encephalitis:
- Indigenously developed Vaccine by India
- The vaccine has been jointly developed by scientists of National Institute of Virology (NIV), Indian Council of Medical Research (ICMR) and Bharat Biotech Ltd.
Scope of Disease:
- It predominantly affects population below 15 years.
- There is seasonal and geographical variation in the causative organism.
- JEV has its endemic zones running along the Gangetic plane including states of UP (east), Bihar, West Bengal and Assam, and parts of Tamil Nadu.
- Government Action- Japanese Encephalitis is part of disease covered under Mission Indradhanush India’s Universal Immunization Programme (UIP).
Mains Perspective:
- What are government measures regarding controlling spread of Encephalitis in country and what further need to be done
- Hints:
- Preventive Measure
- Disease is usually controlled only after the arrival of monsoon rains.
ACUTE ENCEPHALITIS SYNDROME
15, Jun 2019
Context:
- Bihar has recorded 188 cases of acute encephalitis syndrome, with 45 deaths, since January. The cause of death in most this year has been attributed to hypoglycaemia (low blood sugar level).
What is Acute Encephalitis Syndrome (AES)?
- -AES affects central nervous system, mostly in children and young adults.
- -It starts with high fever,then hampers neurological functions causing mental disorientation, seizure, confusion, delirium, coma.
- The disease outbreak is usually reported during monsoons (June- October). But the incidence is also reported during April-June in Bihar.
- Locally known as Chamki Bukhar in the state.
What Causes AES?
- It can be caused by virus, bacteria, fungi, and a range of agents.
- Japanese encephalitis (JE) virus is the most common cause of AES in India, with union health ministry estimate attributing 5-35 per cent cases due to JE.
- But the syndrome is also caused by scrub typhus, dengue, mumps, measles, even Nipah or Zika virus.
- In several cases though the cause of AES remains clinically unidentified.
Status of AES in India:
- -According to National Vector Borne Diseases Control Programme (NVBDCP), 10,485 AES cases were diagnosed in 2018 with 632 deaths across 17 states.
- India records fatality rate at 6 per cent in AES, but the fatality rises to 25 per cent amongst children.
- Bihar, Assam, Jharkhand, Uttar Pradesh, Manipur, Meghalaya, Tamil Nadu, Karnataka, and Tripura are worst affected.
Relation between hypoglycaemia, children and AES:
- Bihar government officials claim AES is a syndrome not disease, and cause of death in these children was found to be prolonged hypoglycaemia that witnessed delayed treatment. In 2014 research paper titled ‘Epidemiology of Acute Encephalitis Syndrome in India: Changing Paradigm and Implication for Controlʼ, co-authored by six researchers, a parallel was drawn between
- Muzaffarpur and Vietnamʼs Bac Giang province where undernourished.
- Children were suffering from AES and hypoglycaemia that coincided with litchi orchards in neighbourhood.
- “The possible association with some toxin in litchi or in environment need to be documented. Methylene cyclopropyl glycine (MCPG) which has been known to be a content of litchi fruit has been shown to cause hypoglycaemia in experimental animals,” the study stated. Several children in Muzaffarpur who suffer from AES before 2014 have a history of visit to litchi orchards, the study found.
- The impact is worse on undernourished children who remain hungry for several hours.
PNEUMOCOCCAL VACCINATION LAUNCHED
13, Jun 2019
Why in News:
- It will help babies with low birth weight and reduce Infant Mortality Rate.
Background:
- In a step towards reducing Infant Mortality Rate, the State has rolled out a pneumococcal vaccination programme. “Babies weighing less than 1.5 kg are admitted to SNCUs.Post- discharge, some of them develop respiratory infection and pneumonia and die in two or three months. One of the common causes of infant mortality is respiratory tract infection and pneumonia. In fact, pneumonia still tops the list for under-five mortality,” Neonatal Intensive Care Unit, and registrar of Institute of Child Health.
- It was to prevent pneumonia and meningitis that an initiative to offer pneumococcal vaccination
Pneumococcal Vaccination:
- To cover babies with very low birth weight and discharged from Special Newborn Care Units (SNCU) in medical college hospitals, district headquarters hospitals and sub-district hospitals. The recommended schedule: first dose at six weeks, second dose at 10 weeks, and third at 14 weeks, and a booster dose at 15 months.
- The vaccines were made available through the Tamil Nadu Medical Services Commission On an average, 490 to 530 babies are admitted to our Neonatal Intensive Care Unit every month. Of this, 30 to 40% are pre-term. These are high risk babies and are prone to infections. Vaccination would provide good protection to them against pneumonia, pneumococcal meningitis, sinusitis and ear discharge.
NIPAH VIRUS CASE IN KERALA
07, Jun 2019

Why in News:
- A youth from Ernakulam district in Kerala has tested positive for the Nipah virus infection (a year after a similar outbreak in Kerala had claimed 17 lives).
What is the Nipah virus infection?
- Cause – The natural host of the Nipah virus are fruit bats of the Pteropodidae family and Pteropous genus, widely found in South and South East Asia.
- However, the actual source of the current infection is not yet known.
- Scientists are currently working on finding the epidemiological link of the outbreak. Transmission – The infection is generally transmitted from animals to human beings, mainly from bats and pigs.
- Human-to-human transmission is also possible, and so is transmission from contaminated food.
- Effect – Nipah virus causes a so far incurable infection in human beings, which can sometimes be fatal.
- Patients either show no symptoms of the infection (asymptomatic infections), thereby making it difficult to detect.
- Otherwise, patients develop acute respiratory problems, or encephalitis that often becomes fatal. The World Health Organization (WHO) says the infection has been found to be fatal in 40% to 75% of the infected patients. There is no treatment available as of now, either for humans or animals, nor any vaccine.
What are the previous incidents of infection?
- Nipah virus infections were first identified in 1999 in Malaysia.
- From then on infections have been detected quite frequently in Bangladesh.
- Kerala – There have been a few incidents of infection in India earlier, apart from the 2018 outbreak in Kerala.
- The 2018 outbreak was confined to two districts of Kerala, Kozhikode and Malappuram. Studies have revealed that a particular kind of fruit bat, Pteropus spp, was most likely the source of human infection in 2018.
- Research suggested that this particular strain might have been circulating in the local bat population. The newly detected case in Kerala is believed to have actually been a result of intensified preventive and containment efforts after last year’s outbreak.
- The increased awareness and vigilance in the community has helped in early detection this time. Elsewhere in India – The first outbreak was in 2001 in Siliguri, West Bengal.
- More than 30 people were hospitalised with suspected infection then.
- Another outbreak happened in 2007 in Nadia of West Bengal, with over 30 cases of fever with acute respiratory distress and/or neurological symptoms.
- Notably, five of them turned out to be fatal.
Who are Potentially at Risk?
- Transmission to 18 contacts last year and the two health-care workers this year has been only through the human-to-human route.
- As of now, the current outbreak is likely localised, like last year’s.
- More people showing symptoms are being screened and so are people in physical contact with them.
- Those with exposure to body fluids (saliva, urine, sputum) of infected patients had higher risk for asymptomatic infections, than those who only had physical contact with the infected patients.
What are the measures taken?
- The National Institute of Virology (NIV) advised extreme care for healthcare workers and caregivers.
- These include providing double gloves, fluid-resistant gown, goggles, face shields, closed shoes and similar other protective gear.
- Currently, steps are being taken to prevent the spread of the disease by tracing the contacts, setting up isolation wards and public engagement.
What is the Way Forward?
- Containing the spread of the Nipah virus is important as the mortality rate was 89% last year. The recurrence of the infection possibly suggests that the virus is in circulation in fruit bats. Analysing the evolutionary relationships, a study found 99.7-100% similarity between the virus in humans and bats.
- The confirmation of the source and the recurrence mean that Kerala must be alert to the possibility of frequent outbreaks. It is high time that the state takes continuous monitoring and surveillance for the virus in fruit bats. One reason for the failure in not doing so till now could be the absence of a public health protection agency. The government has been in the process of formulating it for over 5 years now, to track such infective agents before they strike. The state should also equip the Institute of Advanced Virology in Thiruvananthapuram to undertake testing of dangerous pathogens.
NIPAH IS CONFIRMED, PRECAUTIONS IN PLACE
05, Jun 2019

Why in News:
- Nearly a year after a Nipah outbreak in Kozhikode and Malappuram, the deadly disease has resurfaced in Kerala with the confirmation of the infection.
Details:
- The test results have come from the National Institute of Virology (NIV), Pune, and it is positive for Nipah.
- The health authorities have made elaborate arrangements and medicines are in stock.
- The Health Ministry said the team, comprising an epidemiologist, had been sent to the State to conduct contact tracing for early detection of suspects and review of isolation facilities.
What is Nipah Virus?
- According to WHO, the Nipah virus infection is a newly emerging zoonosis, that is, a disease transmitted from animals to humans. The virus belongs to a new genus termed Henipavirus (subfamily Paramyxovirinae).
- The natural host of the virus are fruit bats belonging to the family Pteropodidae. In 2004, humans were affected after eating the date palm contaminated by infected fruit bats. Pigs can also act as intermediate hosts.
What are the symptoms in humans?
- The symptoms of Nipah are similar to that of influenza: fever, muscle pain, and respiratory problems.
- Inflammation of the brain can also cause disorientation. Late onset of Encephalitis can also occur. Sometimes a person can have an asymptomatic infection, and be a carrier of Nipah and not show any symptoms.
Are there Any Vaccines?
- Currently, there are no vaccines for both humans and animals. Intensive supportive care is given to humans infected by Nipah virus.
- According to WHO, ribavirin can reduce the symptoms of nausea, vomiting, and convulsions associated with the disease.
- Individuals infected need to be hospitalised and isolated. Special care should be taken to prevent human-to-human transmission. Surveillance systems should be established to detect the virus quickly and to initiate appropriate control measures.
IMMUNOTHERAPY BOOSTS SURVIVAL CHANCES FOR LUNG CANCER PATIENTS
03, Jun 2019
Why in News:
- An immunotherapy treatment helped significantly boost survival rates among patients suffering from advanced lung cancer, according to the results of a clinical trial cited by researchers.
Details:
- Almost 25% of patients who received the drug Pembrolizumab and had not previously received chemotherapy were alive after five years. The figure dropped to just over 15% for patients who had previously received chemotherapy. Unlike chemotherapy, immunotherapy works by leveraging the body’s own immune system to fight disease.
More effective T-cells
- The drug acts by turning off a brake in the immune system, a protein called PD-1, which then allows cancer-fighting T-cells to attack faster and more effectively.
- Moving forward, team would like to identify other biomarkers to further improve survival rates.
Biomarker
- A biomarker is a measurable indicator of the severity or presence of some disease state.
- More generally a biomarker is anything that can be used as an indicator of a particular disease state or some other physiological state of an organism.
CHINA LAYING DOWN GENE EDITING RULES
02, Jun 2019

Why in News:
- In an attempt to make babies immune to infection by the human immunodeficiency virus (HIV) China, used a clinically untested gene editing tool
(CRISPR-Cas9) to modify a particular gene
Details:
- In 2012, scientists discovered that CRISPR is a key part
of the “immune system”. - When a virus enters bacteria, it fights back by cutting up the virus’s DNA. This kills the virus but bacteria store some of the DNA. The next time there is an invasion, bacteria produce an enzyme called Cas9 which matches the stored fingerprints with that of the invaders. If it matches, Cas9 can snip the invading DNA.
- The CRISPR-Cas9 gene editing tool thus has two components
- • A short RNA sequence that can bind to a specific target of the DNA and
- • The Cas9 enzyme which acts like a molecular scissor to cut the DNA.
- Once the DNA is cut, the natural DNA repair mechanism is utilised to add or remove genetic material or make changes to the DNA.
- CCR5 gene also helps to protect the lungs, the liver and the brain during certain serious infections and chronic diseases. The gene is known to prompt the immune system to fight the influenza virus in the lungs.
- China posted the draft regulation requiring researchers to obtain prior approval from the government before undertaking clinical trials. Those found violating the rules will be punished and this includes a lifetime ban on research. China is now all set to introduce gene-editing regulation.
CRISPR-Cas9:
- CRISPR is a dynamic, versatile tool that allows us to target nearly any genomic location and potentially repair broken genes. It can remove, add or alter specific DNA sequences in the genome of higher organisms.
- CRISPR (Clustered Regularly Interspaced Short Palindromic Repeats)are sections of DNA and are sections of genetic code containing short repetitions of base sequences followed by spacer DNA segments.
- CAS-9 (CRISPR-associated protein 9) is an enzyme. It uses a synthetic guide RNA to introduce a double strand break at a specific location within a strand of DNA.
- It is a system used by bacterial cells to recognize and destroy viral DNA as a form of adaptive immunity.
- CRISPR scans the genome looking for the right location and then uses the Cas9 protein as molecular scissors to snip through the DNA.
- Cas9 endonuclease – guide RNAs to direct it to a particular sequence to be edited. The genetic sequence of the RNA matches the target sequence of the DNA that has to be edited.
- When Cas9 cuts the target sequence, the cell repairs the damage by replacing the original sequence with an altered version.
- Unlike other gene-editing methods, it is cheap, quick, easy, safer and more accurate to use because it relies on RNA–DNA base pairing, rather than the engineering of proteins that bind particular DNA sequences.
E-Cigarettes Pose Public Health Risk, Says ICMR
01, Jun 2019

Why in News:
- The Indian Council of Medical Research (ICMR) has warned of a potential public health disaster if action was not taken to completely prohibit and dissuade the use of Electronic Nicotine Delivery Systems (ENDS) or e-cigarettes.
Details:
- The nicotine delivered by these devices adversely affect almost all systems in a human body.
- E-cigarette use adversely affects the cardiovascular system, impairs respiratory immune cell function and airways in a way similar to cigarette smoking and is responsible for severe respiratory disease.
- It also poses risk to foetus, infant, and child brain development
Harmful effects
- “Use of e-cigarettes has documented adverse effects on humans which include DNA damage; carcinogenesis; cellular, molecular and immunological toxicity; respiratory, cardiovascular and neurological disorders and adverse impact on foetal development and pregnancy,’’ Given the harmful health effects e-cigarettes pose to users, as well as passive exposure, failure to make appropriate interventions at the right time could lead to a public health disaster in India.
Urges complete ban
- There are more than 460 different e-cigarette brands with varying configurations of nicotine delivery available in the market, according to the ICMR.
- The ICMR has recommended complete prohibition on ENDS or e-cigarettes in India in the greater interest of protecting public health.
- E-cigarettes also open a gateway for new tobacco addiction, which is a potential threat to the country’s tobacco control laws and ongoing tobacco control programmes and efforts
ICMR
- ICMR is India’s apex scientific body for the formulation, coordination and promotion of biomedical research. It was established in 1911 as Indian Research Fund Association (IRFA) making it one of oldest and largest medical research bodies in the world.
- The ICMR functions under Department of Health Research, Ministry of Health and Family Welfare. It is headquartered in New Delhi.
BURNOUT A MEDICAL CONDITION, SAYS WHO
28, May 2019

Why in News:
- The World Health Organization has for the first time recognised “burn-out” in its International Classification of Diseases (ICD), which is widely used as a benchmark for diagnosis and health insurers.
Details:
- The decision, reached during the World Health Assembly in Geneva, could help put to rest decades of debate among experts over how to define burnout, and whether it should be considered a medical condition. WHO defines burn-out as “a syndrome conceptualised as resulting from chronic workplace stress that has not been successfully managed?”
Three dimensions:
- The syndrome was characterised by three dimensions: “1) feelings of energy depletion or exhaustion; 2) increased mental distance from one’s job, or feelings of negativism or cynicism related to one’s job; and 3) reduced professional efficacy.”
- Burn-out refers specifically to phenomena in the occupational context and should not be applied to describe experiences in other areas of life,” This is the first time” burnout has been included in the ICD classification. The ICD-11, which is to take effect in January 2022, contains several other additions, including classification of “compulsive sexual behaviour” as a mental disorder, although it stops short of lumping the condition together with addictive behaviours. It does however for the first time recognise video gaming as an addiction, listing it alongside gambling and drugs like cocaine.
- The updated list removes transgenderism from its list of mental disorders meanwhile, listing
it instead under the chapter on “conditions related to sexual health”.
ICD:
- ICD is the international standard diagnostic tool for epidemiology, health management and clinical purposes. Its full official name is International Statistical Classification of Diseases and Related Health Problems.
- It is maintained by WHO and is revised periodically.
- It provides common language that allows health professionals to share health information across the globe. It contains around 55,000 unique codes for injuries, diseases and causes of death.
NHA TO COLLABORATE WITH CANCER GRID
24, May 2019

Why in News:
- National Health Authority (NHA) and National Cancer Grid (NCG) have signed an MoU under the Ayushman Bharat- Pradhan Mantri Jan Arogya Yojana (AB-PMJAY).
Details:
- The main objective of this collaboration includes developing uniform standards of patient care for prevention, diagnosis and treatment of cancer; providing specialised training and education in oncology, and facilitating collaborative basic, translational and clinical research in cancer,”
- “The partnership with the National Cancer Grid will bring in experts to enhance the cancer care services provided under AB-PMJAY.”
- The NHA and NCG will now jointly review existing cancer treatment packages, pricing of services, and standard treatment workflows covered under the AB-PMJAY, and
- plug-in necessary gaps to ensure enhanced quality of cancer care.
- The NCG will work closely with the NHA to rationalise payment rates for different benefit packages and treatment/diagnosis plans, and also explore mechanisms to signal the right incentives to providers to ensure quality through pricing mechanisms.
Aayusman bharat
- Creating a network of health and wellness infrastructure across the nation (for primary health care services). Provide insurance cover to minimum 40% of India’s total population (for secondary and tertiary healthcare services).
- Beneficiaries of heath insurance under the scheme will include 50 crore economically weak citizens of India as defined in the social, economic and ethnic census 2011 database. It will cover both rural (8.03 crore) and urban (2.33 crore) families. Ayushman Bharat will subsume the existing Rashtriya Sawasthya Bima Yojna, launched in 2008 and the Senior Citizens Health Insurance Scheme. It will provide a benefit cover of Rs 5 lakh/year/family.
- Expenses incurred will be shared between Centre and States in 60:40 ratio.
- The Government aims to open 5 lakh health and wellness centre by 2022 that will be equipped to treat various diseases. Cashless benefits will be allowed from any public or private empanelled hospitals. Such empanelled hospitals will have ‘Ayushman Mitra’ to assist patients. Benefits can be availed from any place in India and no hospital can refuse treatment under this scheme.
WHO UNVEILS PLAN TO TACKLE SNAKEBITE
24, May 2019

Why in News:
- The World Health Organization unveiled a new strategy to dramatically cut deaths and injuries from snakebites, warning a dearth of antivenoms could soon spark a “public health emergency”.
Details:
- Each year, nearly three million people are bitten by poisonous snakes, with an estimated 81,000-138,000 deaths.
- Another 4,00,000 survivors suffer permanent disabilities and other after-effects, according to WHO figures.
- WHO, which two years ago categorised “snakebite envenoming” as a Neglected Tropical Disease, presented a strategy aimed at cutting snakebite-related deaths and disabilities in half by 2030.
- An important part of the strategy is to significantly boost production of quality antivenoms, WHO said.
- The UN agency called for “the restoration of a sustainable market for snakebite treatment”, insisting on the need for a 25% increase in the number of manufacturers. It plans a pilot project to create a global antivenom stockpile.
Neglected Tropical Diseases
- The World Health Organization (WHO) defines the Neglected Tropical Diseases (NTDs) as- a diverse group of communicable diseases that prevail in tropical and subtropical conditions in 149 countries affect more than one billion people and cost developing economies billions of dollars every year .
- Major NTDs are: Buruli ulcer, Chagas disease, Dengue and Chikungunya, Dracunculiasis (guinea-worm disease), Echinococcosis, Foodborne, Human African trypanosomiasis (sleeping sickness), Leishmaniasis (Kala-azar), Leprosy (Hansen s disease), Lymphatic filariasis, Mycetoma, chromoblastomycosis and other deep mycoses, Onchocerciasis (river blindness), Rabies, Scabies and other ectoparasites,
Why are some tropical diseases called “neglected”?
- The people who are most affected by these diseases are often the poorest populations, living in remote, rural areas, urban slums or conflict zones. Neglected tropical diseases persist under conditions of poverty and are concentrated almost exclusively in impoverished populations in the developing world.
- Need for and significance of R&D into neglected tropical diseases:
- The need for drugs for neglected diseases and also for drug R&D is high in India. The country tops the number of cases for 11 different neglected tropical diseases such as lymphatic filariasis, visceral leishmaniasis, trachoma, tapeworm, roundworm, hookworm, whipworm, dengue and leprosy.
In 2017, there were around 2.8 million new cases of TB, which brought down the global decline of TB. One third of all TB deaths worldwide happen in India.
STUDY ON DIABETES WARNS LACK OF AWARENESS & CONTROL A WORRY
21, May 2019

Why in News:
- Only half the Indian adults in the most productive age group (15-49 years) are aware that they ail from diabetes and only one-fourth of those diagnosed and treated have their blood sugar under control – says a study carried out by the Public Health Foundation of India (PHFI), Harvard T.H. Chan School of Public Health, Madras Diabetes Research Foundation, Heidelberg Institute of Global Health, University of Birmingham and University of Gottingen.
Background:
- Diabetes was defined as blood glucose (BG) ≥ 200 mg/dL if not fasted and ≥ 126 mg/dL
if fasted or reporting to have diabetes.
Diabetes
- Diabetes mellitus (DM) – Commonly referred to as diabetes, is a group of metabolic disorders in which there are high blood sugar levels over a prolonged period.
- Most common types of Diabetes Mellitus are as follows
- Type 2 diabetes – A chronic condition that affects the way the body processes blood sugar (glucose)
- Type 1 diabetes – A chronic condition in which the pancreas produces little or no insulin.
- Prediabetes – A condition in which blood sugar is high, but not high enough to be type 2 diabetes.
- Gestational diabetes – A form of high blood sugar affecting pregnant women. Diabetes insipidus – It occurs when the body can’t regulate how it handles fluids. The condition is caused by a hormonal abnormality and isn’t related to diabetes.
- In addition to extreme thirst and heavy urination, other symptoms may include getting up at night to urinate, or bed-wetting.
- Depending on the form of the disorder, treatments might include hormone therapy, a low- salt diet and drinking more water.
Cause of concern:
- Diabetes is a “high maintenance” disease that leads to severe damage to the heart, kidneys and eyes apart from risk of gangrene if mismanaged. Given the state of the public health system in the country, and the fact that the poor have to pay for healthcare, the findings must be treated as a distress signal on an urgent basis.
- Given that people in rural areas and poorer communities in cities are unable to access care earlier, they would be more prone to advanced complications such as renal failure and blindness due to retinopathy. Since 70% of the population lives in rural areas, even a small increase in percentage of people suffering from diabetes adds up to a large number of people who need sustained medical attention but have access to poor health services.
Underlying causes:
-
For many poorer people in cities, nutritionally well-balanced food may not be within their
means. Eating “junk food” is thus not a matter of choice or taste as much as affordability. - Higher income levels, less physically demanding occupations and increased availability of mechanised transport and household appliances among urban dwellers to possibly explain the higher incidence of the disease in urban areas.
- The pressure of commuting long distances to work and the need to use the public transport system is also not a matter of choice for urban poor. These issues lead to the build-up of stress—another factor that is among the causes of the disease.
- Asian Indians progress faster through the pre-diabetes stage than those of other ethnic groups. Also, as in other countries where diabetes is spreading rapidly, in India too, recreational physical activity is very low, more so, among women from all sections.
- People living in urban areas have access to diabetes care services and can afford the associated out-of-pocket expenditure. However, people living in semi-urban and rural areas do not have access to diabetes centres or clinics that provide comprehensive care.
- The other reasons for this shift could be the increased awareness of healthy practices among affluent sections, which means they are engaging in physical activity and making necessary dietary changes to keep non communicable diseases at bay.
Way Forward:
Conclusion:
- Infectious diseases remain the largest concern in developing countries. However, non- communicable diseases like diabetes (known appropriately as the silent killer) are spreading at a frightening rate. In the 21st century, if we are not to sentence large sections of the population to a half-life, we must act quickly and in concert
AI PROJECT EYES EARLY STAGE DIABETIC RETINOPATHY
14, May 2019

Why in News:
- Early stage diabetic retinopathy has been detected using artificial intelligence (AI) at civic- run dispensaries at mumbai.
Background:
- The unique project is being implemented by the Aditya Jyot Foundation for Twinkling Little Eyes (AJFTLE) and, in a span of eight months, nearly 1,300 diabetes patients have been screened on a retinal imaging device attached to a smartphone.
Diabetic retinopathy:
- Diabetic retinopathy is the commonest diabetic eye disease; it damages blood vessels in light-sensitive tissue at the back of the retina.
Symptoms:
- Spots or dark strings floating in your vision (floaters)
- Blurred vision
- Dark or empty areas in your vision Vision loss
- Fluctuating vision
- Vision loss
- Impaired color vision
Causes: / Diabetic retinopathy
- Over time, too much sugar in your blood can lead to the blockage of the tiny blood vessels that nourish the retina, cutting off its blood supply. As a result, the eye attempts to grow new blood vessels. But these new blood vessels don’t develop properly and can leak easily.
- There are two types of diabetic retinopathy:
- Early diabetic retinopathy. In this more common form — called nonproliferative diabetic retinopathy (NPDR) — new blood vessels aren’t growing (proliferating).
- When you have NPDR, the walls of the blood vessels in your retina weaken. Tiny bulges (microaneurysms) protrude from the vessel walls of the smaller vessels, sometimes leaking fluid and blood into the retina. Larger retinal vessels can begin to dilate and become irregular in diameter, as well. NPDR can progress from mild to severe, as more blood vessels become blocked.
- Nerve fibers in the retina may begin to swell. Sometimes the central part of the retina (macula) begins to swell (macular edema), a condition that requires treatment.
- Diabetic retinopathy can progress to this more severe type, known as proliferative diabetic retinopathy. In this type, damaged blood vessels close off, causing the growth of new, abnormal blood vessels in the retina, and can leak into the clear, jelly-like substance that fills the center of your eye (vitreous).
- Eventually, scar tissue stimulated by the growth of new blood vessels may cause the retina to detach from the back of your eye. If the new blood vessels interfere with the normal flow of fluid out of the eye, pressure may build up in the eyeball. This can damage the nerve that carries images from your eye to your brain (optic nerve), resulting in glaucoma.
- Anyone who has diabetes can develop diabetic retinopathy. Risk of developing the eye condition can increase as a result of:
- Duration of diabetes — the longer you have diabetes, the greater your risk of developing diabetic retinopathy
- Poor control of your blood sugar level
- High blood pressure
- High cholesterol
- Pregnancy Tobacco use
- As a part of the AI project, technicians from the Aditya Jyot Foundation visit civic dispensaries along with Remedio Fundus on Phone, a portable device attached to a smartphone equipped with retinal imaging.
- After the patient’s eye images are clicked, the AI on the device screens them for signs of diabetic retinopathy, and prompts technicians on whether they should be referred to a hospital or not. If the image is unclear, the device also prompts a retake of the picture.
Advanced diabetic retinopathy:
Risk factors:
AI role :
India Facing Critical Shortage Of Healthcare Providers: Who
11, May 2019

Why in News:
- Despite the health sector employing five million workers in India it continues to have low density of health professionals.
Details:
- It is lower than those of Sri Lanka, China, Thailand, United Kingdom and Brazil, according to a World Health Organisation
- This workforce statistic has put the country into the “critical shortage of
- healthcare providers” category. Bihar, Jharkhand, Uttar Pradesh and
- Rajasthan are the worst hit while Delhi, Kerala, Punjab and Gujarat compare Southeast Asia needs a 50% increase in healthcare manpower to achieve universal health coverage by 2030. India faces the problem of acute shortages and inequitable distributions of skilled health workers as have many other low- and middle-income countries,’
New courses needed
- The need of the hour is to design courses for different categories of non-physician care providers.
- Competencies should be valued and reform must be brought in regulatory structures to provide flexibility for innovations,
- Data on the prevalence of occupational vacancies in the health care system in India overall is
- Government statistics for 2008, based on vacancies in sanctioned posts showed 18% of primary health centres were without a doctor, about 38% were without a laboratory technician and 16% were without a pharmacist,”
- The health workforce in India comprises broadly eight categories, namely: doctors (allopathic, alternative medicine); nursing and midwifery professionals; public health professionals (medical, non-medical); pharmacists; dentists; paramedical workers (allied health professionals); grass-root workers (frontline workers); and support
World Health Organization
- WHO is a specialised agency of UN
- It is concerned with international public health
- It acts as coordinating authority on international public health Established in 1948
- It succeeded the Health Organization, which was an agency of the League of HQ: Geneva, Switzerland
- India is a founder member of WHO.
- It is a member of UN Development Group (UNDP).
- WHO flag features the Rod of Asclepius as a symbol for healing
National Health Mission
- The National Health Mission (NHM) envisages achievement of universal access to equitable, affordable & quality health care services that are accountable and responsive to people’s needs. The National Health Mission seeks to ensure the achievement of the following indicators. Reduce Maternal Mortality Rate (MMR) to 1/1000 live births
- Reduce Infant Mortality Rate (IMR) to 25/1000 live births Reduce Total Fertility Rate (TFR) to 1
- Prevention and reduction of anaemia in women aged 15–49 years
- Prevent and reduce mortality & morbidity from communicable, non-communicable; injuries and emerging Reduce household out-of-pocket expenditure on total health care expenditure. Reduce annual incidence and mortality from Tuberculosis by half
- Reduce prevalence of Leprosy to <1/10000 population and incidence to zero in all districts Annual Malaria Incidence to be <1/1000
- Less than 1 per cent microfilaria prevalence in all districts
- Kala-azar Elimination by 2015, <1 case per 10000 population in all blocks
COMFORT FOOD LEADS TO MORE WEIGHT GAIN DURING STRESS: STUDY
29, Apr 2019

Why in News?
- Indulging in high-calorie ‘comfort’ foods when stressed can lead to more weight gain than usual, scientists say.
Details:
- Researchers from the Garvan Institute of Medical Research in
- Australia discovered a molecular pathway in the brain, controlled by insulin, which drives the additional weight gain. Using an animal model, the team showed that a high-calorie diet when combined with stress resulted in more weight gain than the same diet caused in a stress-free environment. “This study indicates that we have to be much more conscious about what we’re eating when we’re stressed
- To understand what controls this ‘stress eating’, the team investigated different areas of the brain in mice. While food intake is mainly controlled by a part of the brain called the hypothalamus, another part of the brain — the amygdala — processes emotional responses, including anxiety. The study showed that when stressed over an extended period and high calorie food was available, mice became obese more quickly than those that consumed the same high fat food in a stress-free environment,”
NPY
- At the centre of this weight gain, the scientists discovered, was a molecule called NPY, which the brain produces naturally in response to stress to stimulate eating in humans as well as mice.
- Without NPY, the weight gain on a high-fat diet with stress was the same as weight gain in the stress-free environment,
- “This shows a clear link between stress, obesity and NPY,
- Under normal conditions, the body produces insulin just after a meal, which helps cells absorb glucose from the blood and sends a ‘stop eating’ signal to the hypothalamus feeding centre of the brain. The scientists discovered that chronic stress alone raised the blood insulin levels only slightly, but in combination with a high-calorie diet, the insulin levels were 10 times higher than mice that were stress-free and received a normal diet.
- The study showed that these prolonged, high levels of insulin in the amygdala caused the nerve cells to become desensitised to insulin, which stopped them from detecting insulin altogether. In turn, these desensitised nerve cells boosted their NPY levels, which both promoted eating and reduced the bodies’ normal response to burn energy through heat.
Vitamin deficiency high among urban adults, says NIN study
24, Mar 2019

Scientists at the ICMR-National Institute of Nutrition (NIN) screened the sub-clinical status of vitamins A, D, B1, B2, B6, B12 and folate among urban adults in the twin cities and they found several vitamin deficiencies and dietary inadequacies hidden under their apparently healthy exterior.
For the first time, explored the blood levels of major vitamins along with dietary intakes of urban adults and explored the homocysteine levels which amplify the chances of non-communicable diseases like heart diseases.
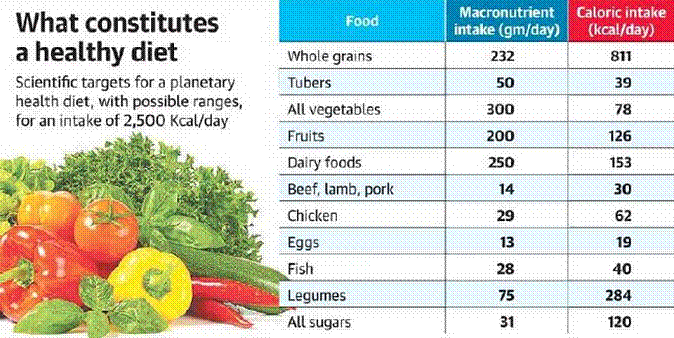
Vitamins:
- Vitamins are organic compounds that are required in small amounts in our diet but their deficiency causes specific diseases.
- Most of the vitamins cannot be synthesized in our body but plants can synthesize almost all of them, so they are considered as essential food factors.
- However, the bacteria of the gutcan produce some of the vitamins required by us.
- All the vitamins are generally available in our diet. Different vitamins belong to various chemical classes and it is difficult to define them on the basis of structure.
- They are generally regarded as organic compoundsrequired in the diet in small amounts to perform specific biological functions for normal maintenance of optimum growth and health of the organism.
- Vitamins are designated by alphabets A, B, C, D, etc. Some of them are further named as sub-groups e.g. B1, B2, B6, B12, etc.
- Vitamin A keeps our skin and eyes healthy.
- Vitamin C helps body to fight against many diseases. Vitamin C gets easily destroyed by heat during cooking.
- Vitamin D helps our body to use calcium for bones and teeth.
- Excess of vitamins is also harmful and vitamin pills should not be taken without the advice of doctor.
- The term “Vitamine” was coined from the word vital + amine since the earlier identified compounds had amino groups.
- Later work showed that most of them did not contain amino groups, so the letter ‘e’ was dropped and the term vitamin is used these days.
- Vitamins are classified into two groups depending upon their solubility in water or fat.
Fat soluble vitamins
- Vitamins which are soluble in fat and oils but insoluble in water are kept in this group. These are vitamins A, D, E and K. They are stored in liverand adipose (fat storing) tissues.
Water soluble vitamins
- B group vitamins and vitamin C are soluble in water so they are grouped together.
- Water soluble vitamins must be supplied regularlyin diet because they are readily excreted in urine and cannot be stored (except vitamin B12) in our body.
| S.No | Vitamin | Deficiency Diseases |
|---|---|---|
| Vitamin A | Night blindness | |
| Vitamin B1 | Beriberi | |
| Vitamin B2 | Ariboflavinosis | |
| Vitamin B3 | Pellagra | |
| Vitamin B5 | Paresthesia | |
| Vitamin B6 | Anemia | |
| Vitamin B7 | Dermatitis, enteritis | |
| Vitamin B9 & Vitamin B12 | Megaloblastic anemia | |
| Vitamin C | Scurvy, Swelling of Gums | |
| Vitamin D | Rickets & Osteomalacia | |
| Vitamin E | Less Fertility | |
| Vitamin K | Non-Clotting of Blood. |
CCR5 Delta 32
07, Mar 2019

Context
- For just the second time since the global epidemic began, a patient appears to have been cured of infection with HIV, the virus that causes AIDS.
About the News:
- This is the second Patient to be cured of HIV AIDS
- Both milestones resulted from bone-marrow transplants given to infected patients. But the transplants were intended to treat cancer in the patients, not HIV.
- The transplants were from a donor with a mutation in a protein called CCR5, which rests on the surface of certain immune cells. HIV uses the protein to enter those cells but cannot latch on to the mutated version.
- CCR5 is the protein that He Jiankui, a scientist in China, claimed to have modified with gene editing in at least two children, in an attempt to make them resistant to HIV — an experiment that set off international condemnation.
About CCR5-Delta 32 Mutation:
- The remarkable research breakthrough that appears to have cured the anonymous “London Patient” of HIV is based on a stem cell transplant involving CCR5-delta 32 homozygous donor cells.
- This is the same treatment that cured Timothy Ray Brown, known as the “Berlin Patient” when he received two stem cell transplants in 2007 and 2008.
- HIV uses the CCR5 protein to enter immune cells, but it can’t latch on to cells that carry the delta 32 mutation. IciStem, a consortium of European scientists studying stem cell transplants to treat HIV infection, has a database of 22,000 donors with this HIV-resistant mutation. About 1% of people of Northern European descent, mainly Swedes, are born with a mutation known as CCR5-delta 32, which “locks ‘the door’ which prevents HIV from entering into the cell. This is only going to work if someone has a virus that really only uses CCR5 for entry. Patient would still be vulnerable to a form of HIV called X4, which employs a different protein, CXCR4, to enter cells.
Brown’s Case:
- Dr Hütter put Brown through an allogeneic stem cell transplant, which involved replacing his immune system with donor hematopoietic stem cells (usually found in bone marrow) so that his immune system could be regenerated, with no malignant cells. Importantly however, the donor he chose carried what is called a CCR5-delta 32 mutation.
Scientists Boost Plant Yield by 40%
07, Jan 2019

Context:
- Researchers have found a way to boost the plant growth genetically.
Details:
- Scientists have confirmed 40% increase in tobacco plant productivity using their genetic shortcut.. The same mechanism could be replicated in other plants such as wheat or soy beans in order to meet demand.
- According to the research, the enzyme ‘Rubisco’, which is a key to carbon fixation process (converting atmospheric carbon into an organic compound, consumed by plants), also acts to fix atmospheric oxygen, converting it into toxic compounds that the plant expends considerable energy eliminating it. This competing process is called photorespiration. The scientists have discovered that implanting bits of algae DNA into the tobacco plant’s cells to create a type of biological shortcut would speed up the process of photorespiration.
- According to them, when a plant uses less energy on photorespiration, it will be able to take that energy and put it into plant growth and plant productivity, rather than using it to metabolise this toxic compound.
New Antibody for Cancer Treatment
03, Oct 2018

- A team of researchers in Spain, Switzerland and the U.S. has homed in on a specific antibody, called the p95HER2-T cell bispecific antibody (TCB), that can successfully guide immune cells, known as lymphocytes, directly to cancerous ones for their targeted killing.
About:
- The immune system has the natural capacity to fight against disseminated disease. To do so more effectively, it must be better equipped to recognize and act against malignant cells. While bispecific antibodies are designed to do just that, they often signpost T cells to healthy ones.
- Among the key hurdles in cancer immunotherapy an emerging approach to cancer medicine is to ensure that these therapeutics only target cancerous cells and not healthy tissue.
- This direct delivery is achieved by p95HER2 protein, which is only located in tumour cells. Not only are they highly specific but they can also hone in on one protein among tens of thousands, in this particular case, p95HER2.
- The study represents a new therapeutic avenue and fresh hope for patients who have ceased to respond to current therapies.
- This novel immune-based approach, can be used to tackle certain HER2+ breast cancers through its exclusive targeting of cancerous cells.
- Each antibody molecule has a bipartite structure containing two protein-binding sites. This means that they can simultaneously attach to immune cells and cancerous ones as well as take the lymphocytes hand-in-hand directly to the malignant cells for their subsequent destruction.
- It is an important step towards ensuring that the immune system can successfully deliver its powerful anti-cancer blows.
- Approximately 10% of patients with HER2-positive breast cancers expressing p95HER2 could stand to benefit from this novel strategy who no longer responded to standard therapies.
- By more precisely matching novel therapy to a particular patient population, we are getting closer to delivering on the true promise of precision medicine.
Delhi Government Official Bags WHO Award
29, Aug 2018

- Delhi government’s additional director of health S.K. Arora has been awarded the prestigious WHO World No Tobacco Day 2018 Award for his extraordinary contribution towards tobacco control.
National Tobacco Control Programme:
- India is the second largest tobacco consuming country in the world with 27 crore users.
- The National Tobacco Control Programme (NTCP) was launched by the Ministry of Health and Family Welfare (MoHFW), Government of India in 2007- 08, during the 11th five year plan, with the following objectives:
- To bring about greater awareness about the harmful effects of tobacco use and about the Tobacco Control Laws.
- To facilitate effective implementation of the Tobacco Control Laws.
- The key activities undertaken under the National Tobacco Control Programme include:
- National Level Public awareness campaigns
- Monitoring, Evaluation and Research.
- Advocacy and inter-sectoral linkages
- Training and capacity building of multiple stakeholders.
- Enforcement of the Tobacco Control Act (COTPA, 2003)
- School Awareness Programmes
- Setting up and expansion of cessation services.
WHO Framework Convention on Tobacco Control (FCTC)
- The WHO Framework Convention on Tobacco Control (WHO FCTC) is the first global public health treaty. It is an evidence-based treaty that reaffirms the right of all people to the highest standard of health.
- The WHO FCTC was developed by countries in response to the globalization of the tobacco epidemic.
- The Treaty was developed by countries in response to the globalization of the tobacco epidemic.
- There are currently 180 Parties to the Convention.
- India has been the forerunner in ratification of this public health treaty and was the 7th Country to ratify the Convention in 2004.
- India provided a leadership role in the negotiations of FCTC and was also the Regional Coordinator for the South-East Asia Region.
- The Conference of the Parties (COP) is the Governing Body of the WHO FCTC and is comprised of all Parties to the Convention.
- It keeps under regular review the implementation of the Convention and takes the decisions necessary to promote its effective implementation, and may also adopt protocols, annexes and amendments to the Convention.
Outcomes:
- As a result of various measures taken by the government, NGOs and civil society organizations, the tobacco use in the country is estimated to have reduced by 81 lakhs and youth consumption of tobacco has also seen marked decrease.
- A 54% relative reduction in prevalence of tobacco use among minors (15-17 years) and 28% reduction in the age group of 18-24 years has been reported
Congo Cube
28, Aug 2018

- The Alliance for International Medical Action, or ALIMA, in collaboration with Securitec, has developed a self-contained treatment unit or a bio-secure emergency room called CUBE, or Cudor Chambre d’Urgence Biosécurisée.
- It allows for quality care with minimal contamination risks, having been developed in the aftermath of the 2014 Ebola outbreak.
Advantages:
- The primary objective is to confine the start of an outbreak by creating a first line of treatment close to a patient’s home.
- As a transportable unit that can be assembled in 90 minutes, its main advantage is that health workers no longer need personal protective equipment as protection is centred around the patient.
- With its transparent walls and external arm entries, medical teams can comfortably ensure continuous monitoring of an infected patient and also adapting treatment from the outside, reducing the risk of contamination.
- The patient also benefits from the transparent walls which allow them to remain in contact with the outside world, again without the risk of contamination.
- As the unit includes air conditioning and air filtration units, it can also be configured as an operating theatre and ‘P4-level’ laboratory for diagnostics and research.
ISRO Telemedicine Nodes for Soldiers in High-Altitude Areas
20, Aug 2018

- The Integrated Defence Staff of the Defence Ministry and the Indian Space Research Organisation (ISRO) signed a memorandum of understanding to set up telemedicine nodes in critical places across the country.
Telemedicine:
- The delivery of healthcare services, where distance is a critical factor, by all healthcare professionals using information and communication technologies for the exchange of valid information for diagnosis, treatment and prevention of disease and injuries, research and evaluation and for the continuing education of healthcare providers, all in the interests of advancing the health of individuals and their communities.”
- Telemedicine Consulting Centre is the site where the patient is present.
- The Telemedicine system consists of an interface between hardware, software and a communication channel to eventually bridge two geographical locations to exchange information and enable tele consultancy between two locations.
- The hardware consists of a computer, printer, scanner, videoconferencing equipment etc. The software enables the acquisition of patient information (images, reports, films etc.). The communication channel enables the connectivity whereby two locations can connect to each other.
- Telemedicine is one of the unique applications of Space Technology for societal benefit. ISRO Telemedicine programme started in 2001 has been connecting remote/rural/medical college hospitals and Mobile Units through the Indian satellites to major specialty hospitals in cities and towns.
Significance:
- Easy access to remote areas
- Using telemedicine in peripheral health set-ups can significantly reduce the time and costs of patient transportation
- Improves communications between health providers separated by distance
- Critical care monitoring where it is not possible to transfer the patient
- Continuing medical education and clinical research
- A tool for public awareness
- A tool for disaster management
- Second opinion and complex interpretations
- The greatest hope for use of telemedicine technology is that it can bring the expertise to medical practices once telecommunication has been established.
- Tele mentored procedures-surgery using hand robots
- Disease surveillance and program tracking
- It provides an opportunity for standardization and equity in provision of healthcare, both within individual countries and across regions and continents.
Oxytocin
20, Aug 2018

Why in news?
- Setting aside its ban on the sale of oxytocin, the Health Ministry has allowed private retail stores to sell the life-saving hormone oxytocin.
Background:
- Recently government banned imports of the hormone oxytocin to stop its misuse in the livestock industry, where activists say it causes hormonal imbalances and shortens the lives of milch animals.
- Later it says that State-owned Karnataka Antibiotics Pvt Ltd will be the only company to manufacture and distribute oxytocin in India from September 1.
Why oxytocin was restricted to other producers?
- The reason for the ban is the misuse of oxytocin in dairy animals, like buffaloes, to increase milk production.
- Daily oxytocin injections would make cattle barren and reduce their lifespans.
- In addition, it claimed that drinking milk from oxytocin-treated cattle led to male impotence, early puberty among women and cancers.
Was the ban the only solution?
- No, the Drugs Technical Advisory Board recommended against a ban, advocating better surveillance instead. A ban might lead to scarcity and high drug prices.
Aspirin May Help Prevent HIV
16, Aug 2018
- An affordable, globally available drug — low-dose aspirin — could help prevent HIV transmission.
Study:
- Researchers tested the effect of aspirin and other anti-inflammatory drugs on HIV target cells in a group of Kenyan women who were at low risk for HIV.
- Transmission of the virus requires a susceptible target cell in the human host. Activated immune cells are more susceptible to HIV infection than resting cells. It is known that inflammation brings activated HIV target cells to the female genital tract.
- The researchers found that Aspirin was the most effective anti-inflammatory drug. It reduced the number of HIV target cells in the female genital tract by 35 per cent.
Impacts:
- This could be a strategy for HIV prevention that is not only inexpensive, but easily accessed globally.
- This could be a affordable and immediately available prevention approach.
- This helps in providing a new tool in the HIV prevention arsenal that would be used together with other approaches to reduce HIV transmission in high-risk populations.
Ebola Virus
30, Jul 2018
Recently new type of Ebola virus has been found in the continent of Africa (Sierra Leone). Researchers found the new virus in the northern Bombali Region.
Background:
It is not yet known whether the new Bombali species of the virus which reserachers say could be transmitted to humans can develop into the deadly Ebola Diseases. The Ebola Outbreak which happen during 2013 in west Africa continent was most devastating and claimed around more than 11,000 Life’s
About Ebola:
- Ebola virus disease (EVD), also known as Ebola Haemorrhagic Fever (EHF) or simply Ebola, is a viral Haemorrhagic fever of humans and other primates caused by ebolaviruses.
- Signs and symptoms typically start between two days and three weeks after contracting the virus with a fever, sore throat, muscular pain, and headaches. Vomiting, Diarrhoea and rash usually follow, along with decreased function of the liver and kidneys. At this time, some people begin to bleed both internally and externally.
- The virus spreads through direct contact with body fluids, such as blood from infected humans or other animals. Spread may also occur from contact with items recently contaminated with bodily fluids.
- Spread of the disease through the air between primates, including humans, has not been documented in either laboratory or natural conditions.
- Semen or breast milk of a person after recovery from EVD may carry the virus for several weeks to months.
- Fruit bats are believed to be the normal carrier in nature, able to spread the virus without being affected by it. Other diseases such as malaria, cholera, typhoid fever, meningitis and other viral Haemorrhagic Fevers may resemble EVD. Blood samples are tested for viral RNA, viral antibodies or for the virus itself to confirm the diagnosis.
Indian Scenario:
The Ebola Outbreak was first recorded in New Delhi and followed by Death which was inevitable so far in Indian Subcontinent Ebola is not a threat.
Formalin
29, Jul 2018

Samples of fish species tested from Chennai have shown positive for formalin. It is a cancer-inducing chemical used illegally to preserve fish.
Why it is used:
- In Fish industry ,formalin or formaldehyde is sprayed on the fish or injected into the fish or the fish is dipped into the solution. This helps keep the fish fresh for a longer time.
- When formalin is used the gills remain red for longer periods.
Formalin:
- A solution of 35 to 40 per cent of water in formaldehyde.
- Formalin is a colourless strong-smelling, toxic, flammable, explosive liquid substance usually used in industry of textiles, plastics, papers, paint, construction, and well known to preserve human corpse.
- It is also used as raw material for organic combination, formaldehyde resin, plastic production, organic material synthesis, disinfection, and anatomic preparation conservation, as fungicide.
- Effective against viruses.
- Effective against mycobacteria so used as an antiseptic in sterilising surgical instruments.
- It’s vapour together with air form explosive compounds.
- Exposure from its gas or vapor can cause irritation to the eyes, nose and respiratory tract, causing sneezing, sore throat, larynx constriction, bronchitis and pneumonia. Multiple exposures can lead to asthma. It can also affect the skin, causing dermatitis or allergic reaction.
- Formalin that was recently found in food, might not give such obvious reactions. However, this substance is known to be a carcinogenic substance, can precipitate cancer. Some other studies also show formalin will cause kidney, liver, and lung problems.
- Formalin will make the fish become stiff, whitish and odourless. Even when cooked, i.e. fried, it will still be stiff.
- Formalin must be disposed though the hazardous chemical waste disposal program.
Auto Immune Disease
29, Jul 2018

- It is a condition in which the immune system of our body mistakenly attacks our blood cells, joints skin etc.,
- Generally immune system can differentiate foreign cells and own cells.
- In this condition, it mistakenly attacks your parts of the body
Causes:
- Exact causes are unknown
- There are 80 different Auto-immune Diseases.
Eat Right Movement
22, Jul 2018

To improve public health in India and combat negative nutritional trends to fight lifestyle diseases FSSAI launched ‘EAT RIGHT MOVEMENT’.
About:
- ‘The Eat Right Movement’, built on two broad pillars of ‘Eat Healthy’ and ‘Eat Safe’, aims to engage, excite and enable citizens to improve their health and wellbeing.
- ‘The Eat Right Movement’ is a holistic and collaborative approach, with stakeholders on both the demand and supply-side.
- On the demand side, the Eat Right Movement focuses on empowering citizens to make the right food choices.
- On the supply side, it nudges food businesses to reformulate their products, provide better nutritional information to consumers and make investments in healthy food as responsible food businesses.
- The Safe and Nutritious Food Initiative – Focused on social and behavioural change around food safety and nutrition at home, school, workplace and on-the-go.
- The Eat Healthy Campaign – focused on reduction of high fat, sugar and salt foods in the diet.
- Food Fortification – focused on promoting five staple foods-wheat flour, rice, oil, milk and salt that are added with key vitamins and minerals to improve their nutritional content.
- The edible oil industry, bakeries and ‘halwais’ committed to phase out trans-fats by 2022 as voluntary commitments.
- Major food companies voluntarily committed to reformulate packaged foods to reduce the level of salt, sugar and saturated fat.
- The food services sector promised to provide healthier food options and introduce menu-labelling.
- The Eat Right Movement Website is an interface between food safety and nutrition experts and citizens. It provides credible and authentic nutrition information including health tips by experts, nutritious recipes, and exciting tools to get a peek into one’s nutritional needs, body indices, learning about nutrition labels, and other resources.
- An AI Powered Chatbot for citizens to answer all questions related to food is part of the website.
- The Eat Right Toolkit to reach out to people at the grass roots level includes a training manual for frontline health workers such as Health and Wellness Centre workers, ASHA and Anganwadi workers etc and engagement material for citizens in rural and aspirational areas, with a special focus on children.
- Resource books on safe and nutritious food such as the Pink Book for homes, The Yellow Book for schools, The Orange Book for workplaces, The Purple Books for eating out, vetted by domain experts are also in place.
The Eat Right Movement brings together three ongoing initiatives of FSSAI
Background:
- In the last 25 years, a major transition in the disease patterns has taken place in India.
- In 1990, more than 60% of all diseases were either infectious (like TB and diarrhoeal diseases), lack of nutrition (like anaemia). These afflictions now account for just 33% of the disease burden.
- Conversely, the contribution of non-communicable diseases like cardiovascular diseases, diabetes, neurological diseases, cancers, etc, has increased from 30% to 55%. The maximum increase has happened in diseases that are linked to an unhealthy diet and lifestyle.
- The country has more people with type-2 diabetes than any other nation.
- There is now an emerging body of scientific studies linking junk food with childhood obesity and the diabetes epidemics.
- In order to combat this draft Food Safety and Standards (Labelling and Display) Regulations, 2018 has been released for comments by the Food Safety and Standards Authority of India (FSSAI) in April, 2018. • It mandate compulsory labelling of salt and introduced a special red labelling for high in fat, sugar. But it was opposed by food industries due to low consumer base for sugar and fat free items.
So FSSAI launched The Eat Right Movement as an awareness generation and voluntary commitment of food industries to give heathy food to consumers.






